I understand why companies develop products for diabetic foot ulcers (DFUs) and venous leg ulcers (VLUs), even though those are NOT the most common wound problems. It’s because the clinical trials needed to satisfy the Food and Drug Administration (FDA) are well defined in those wound models, and so is the market. They can study uncomplicated, easy to heal wounds, which ensures the trials will go well. Unfortunately, it means that the really difficult problems in wound healing will never have products developed for them because the wounds are too hard to heal.
There are several chronic wound types that make my heart sink. They include calciphylaxis, sickle cell ulcers, scleroderma and atrophie blanche. I also seem to have a clinic full of pyoderma gangrenosum. I am ALWAYS on the lookout for something promising to treat them. There will never be randomized, prospective clinical trials (RCTs) to help these patients – we will have to rely on real world data and anecdotal experience using drugs and devices that are FDA cleared for some other indication. This is called “off-label” use, which is perfectly ethical but which often means that the patient’s insurance will not pay for the treatment – using the argument that it is “unproven” for that indication.
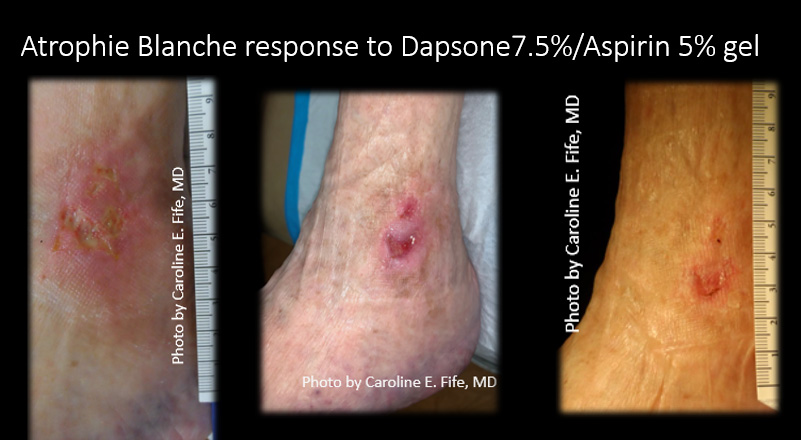
I might have found something helpful for atrophie blanche (AB). The credit is not due to me. Some years ago when I was on the faculty of the University of Texas Health Science Center, Houston, my friend and colleague, dermatologist Adelaide Hebert, MD suggested we try topical Dapsone (Aczone Gel) for atrophie blanche. In 2011, Dr. Erik Maus, Dr. Hebert and I presented a the poster pictured below, about a series of AB patients treated with Aczone Gel at the annual American Academy of Dermatology meeting. The problem is that commercially available Aczone Gel, which is FDA approved for acne, is expensive and prescription drug plans almost never cover it for “off label” use.
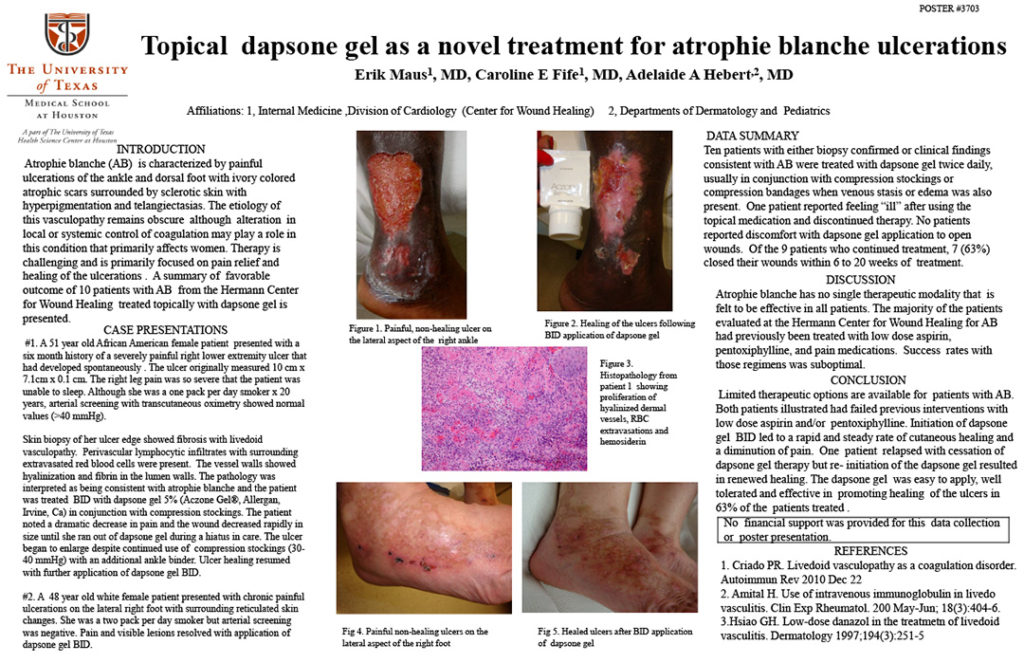
If you wonder exactly what AB looks like, I provide a gallery of photos below. It’s classically described as an ivory white plaque of skin with telangiectasias. It may never ulcerate but when it does, the pain is excruciating. It is commonly associated with venous disease but venous ablation may not improve the ulceration. The mechanism of the ulcerations is poorly understood and since I am NOT a dermatologist, I won’t pretend to be one. The mainstay of therapy is systemic aspirin therapy and compression, but a long list of other systemic drugs have been found somewhat useful including sulfasalazine and pentoxifylline. Prednisone is not useful. These lesions are excruciating (don’t debride them, please!).
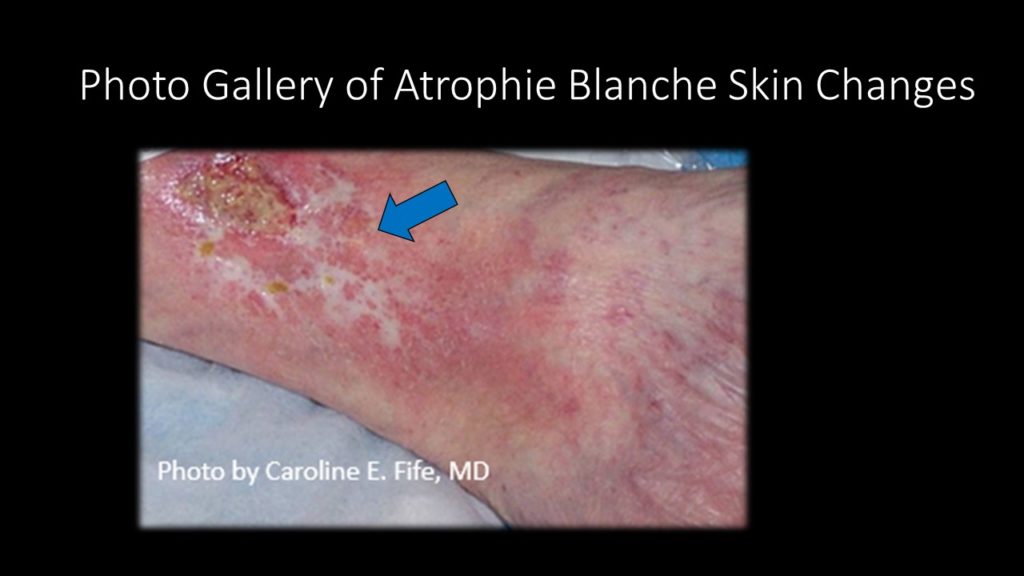
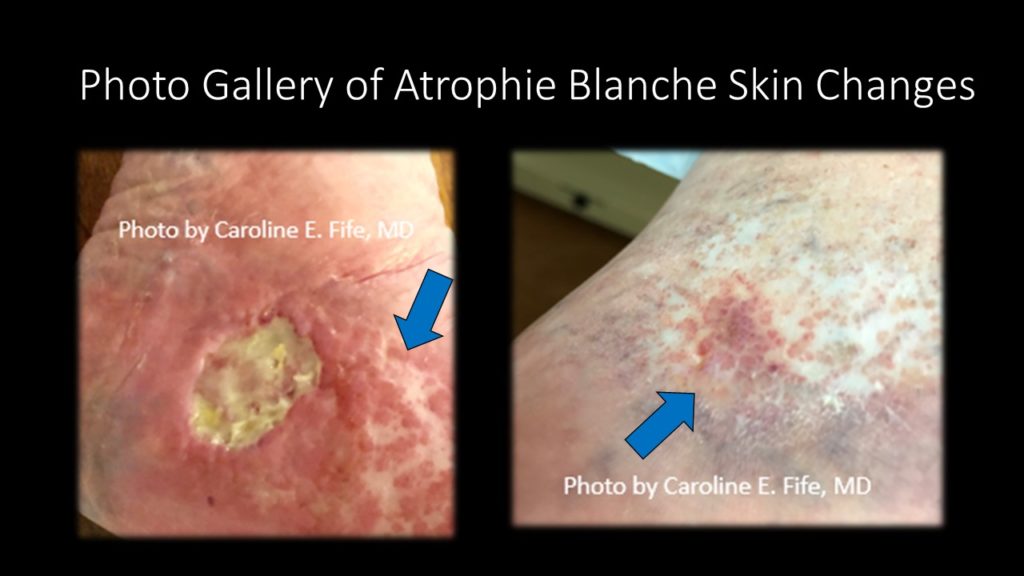
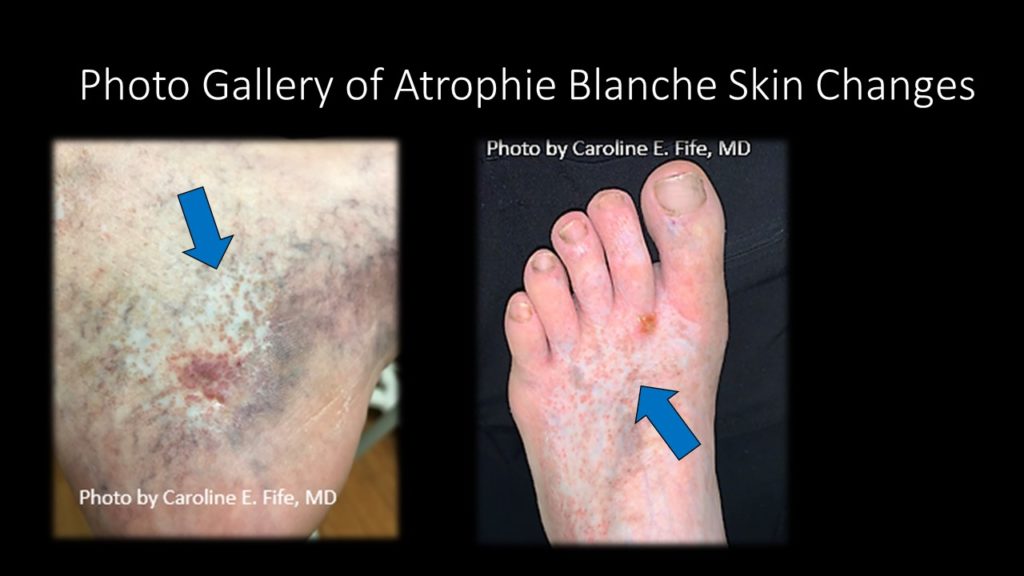
A few months ago, Survam Patel from Smithville Pharmacy contacted me. I’d tried a variety of compounding pharmacies and products, and was less than encouraging on the phone. Over the years I had become frustrated with the challenges involved in ordering compounded treatments for wounds and the variability in pricing, since patients almost always have to pay out of pocket. I told Dr. Pena, the head pharmacist, that if they could help me with my list of “nemesis wounds,” they’d earn my enthusiastic support. So far, we have had some success with atrophie blanche. They compounded topical Dapsone gel, to which we added topical aspirin. It is also possible to add topical anesthetic medication for this painful skin condition. I will keep you posted on how things are going for the other problems. Let me know if you have any secrets for the other “nemesis” conditions.

Dr. Fife is a world renowned wound care physician dedicated to improving patient outcomes through quality driven care. Please visit my blog at CarolineFifeMD.com and my Youtube channel at https://www.youtube.com/c/carolinefifemd/videos
The opinions, comments, and content expressed or implied in my statements are solely my own and do not necessarily reflect the position or views of Intellicure or any of the boards on which I serve.



Love this! Thank you for the good and helpful information!!
Great case! Any idea on the mechanism of action here? Also, brings up the question if there is any use for oral dapsone – it requires monitoring and not without side effects but these patients are typically quite desperate.
Excellent!!!!