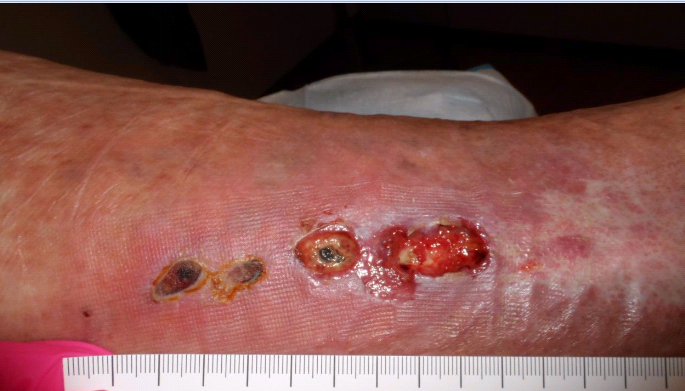
68-year-old with ulcers on the left medial ankle, which began after sclerotherapy with some sort of glue 10 weeks earlier. He has had multiple venous ablation procedures for recurrent venous leg ulcers over the past 15 years. I screened him for arterial disease with skin perfusion pressure and his SPP is normal as is his pulse volume recording; which means this doesn’t have an arterial component.
At first glance the chain of small ulcers looked like some sort of vasculitis, and I suppose you could call it an inflammation of the vessel. The lesions clearly follow the distribution of the saphenous vein. Despite compression bandaging, he continued to have more and more skin breakdown along the distribution of the vessel that had been sclerosed. I asked a plastic surgeon to take him to the operating room, where a lot of non-biological material was removed that looked like tar. The patient is now getting negative pressure wound therapy.
My point is that the pattern of the lesions was important. Pay attention to breakdown that follows the anatomical course of a vessel. But the other reason it matters is that this proves that the occlusion of a vein can lead to breakdown of the overlying skin. This is another “inside to outside” case of tissue necrosis. Just something to think about…
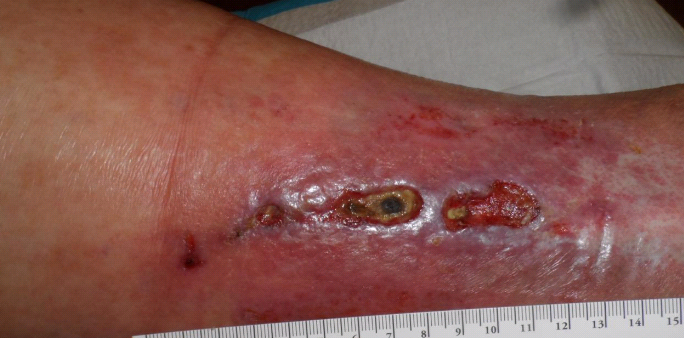
Four Days Later
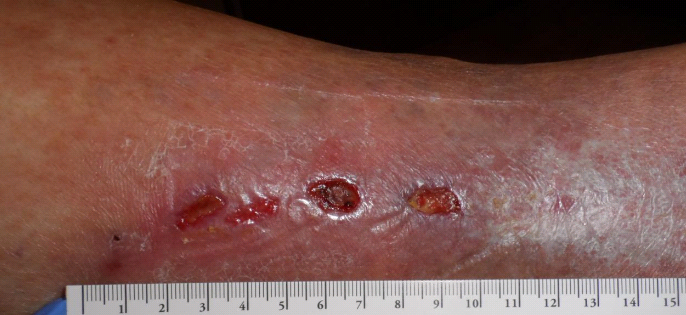
One Week Later
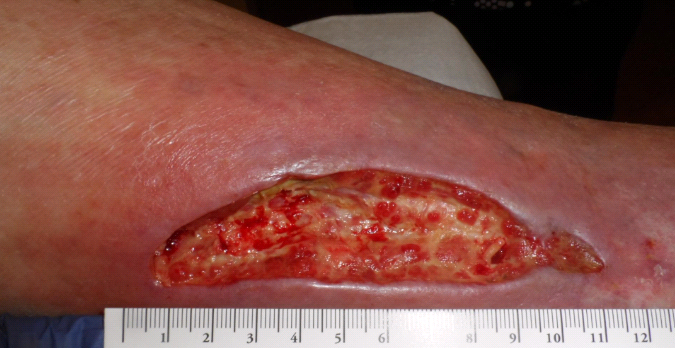 After surgical debridement of the sclerosing agent – 6 weeks after he presented.
After surgical debridement of the sclerosing agent – 6 weeks after he presented.

Dr. Fife is a world renowned wound care physician dedicated to improving patient outcomes through quality driven care. Please visit my blog at CarolineFifeMD.com and my Youtube channel at https://www.youtube.com/c/carolinefifemd/videos
The opinions, comments, and content expressed or implied in my statements are solely my own and do not necessarily reflect the position or views of Intellicure or any of the boards on which I serve.



Have you considered 3CPatch to jumpstart healing? It might be helpful.
Thank you for sharing.
Hey I know this guy. In 1 of those pics the REDness is from adhesives on those telfa pads. Skin on my legs is very sensitive to adhesives.
I’m getting Great Care.