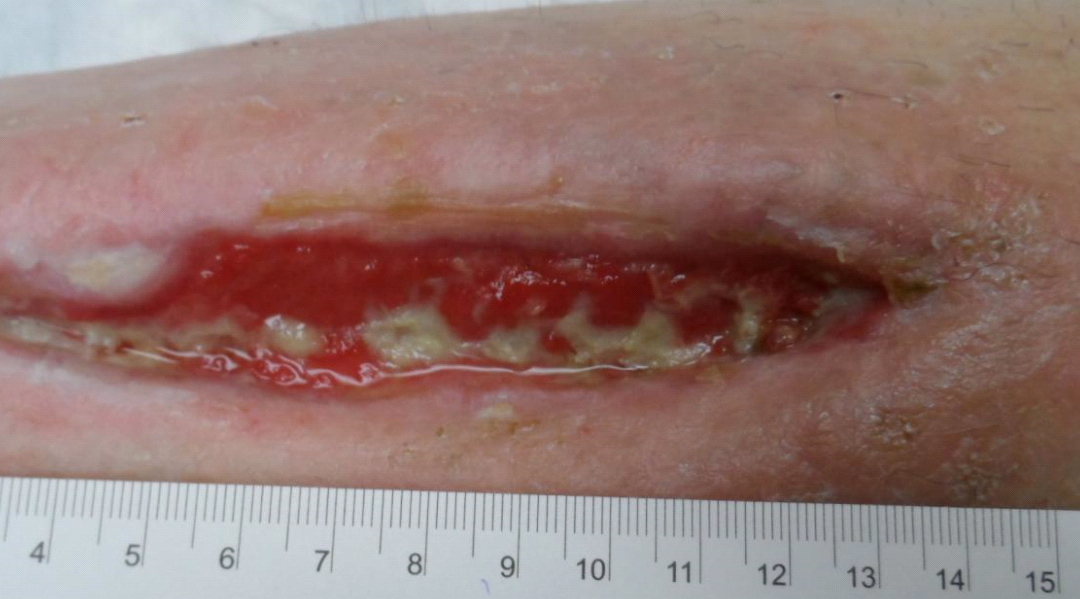
Before Maggots Were Applied
I’d like to frame a discussion about the cost of chronic wound care, through the lens of a wonderful patient. She’s an 80 yo woman with severe peripheral arterial disease and chronic limb ischemia who had already had multiple endovascular interventions in her legs. Diabetes was diagnosed when she developed an abscess on the left anterior shin that lead to acute osteomyelitis of the tibia. Only the anterior tibial artery was patent. The abscess was drained and a local debridement was performed, but this left exposure of necrotic tendons on the shin. Due to her marginal blood flow and the proximity of the only artery perfusing her leg, maggots were used to debride the wound to prepare it for negative pressure wound therapy and a variety of other advanced therapeutics. She had to pay for the maggots since they are not covered by insurance (about $400). These videos of maggots being put on and removed from the wound were actually taken by the patient, and it’s her ungloved hand you see at one point as the dressing is removed. She is a remarkable woman who was a joy to care for.

The Wound After Maggots, NPWT and Other Treatments
Treatments included NPWT (KCI), Dermavest (donated by Aedicell: https://aedicell.com/products/), platelet rich plasma (purchased by the patient from Cytomedix), ACell (https://acell.com/), intravenous antibiotics, topical antibiotics directed by DNA assay (Pathogenius, now Microgen: http://welcome.microgendx.com/), extremely gentle compression therapy, and many so-called “advanced dressings” which are really just routine in a wound center (e.g. collagens, alginates, antimicrobials, etc.). Despite all of those treatments, the real secret weapon was Dr. Kyle Dickson, orthopedist at Methodist Hospital, Houston Medical Center, who is the guru of long bone osteomyelitis. She healed over a 4 year course of care and I am happy to say is walking and swimming again.

The Healed Shin, Four Years After Onset
I bring up her case partly because it’s always fun to see movies of maggots. But, the real reason to talk about this case is to point out that while she did have more than one hospitalization for surgery over 4 years, the majority of her costs were incurred as an outpatient. The reason the majority of costs in wound care are incurred in the outpatient setting is that outpatient care is still mostly a fee for service environment, and patients often take months to heal. Wounds are not a disease, they are a SYMPTOM of a disease (or diseases). Chronic wounds, even when they heal, often return because the diseases they are associated with do not go away. Also, the cost of wound care increases dramatically when there is associated infection.
Maggots Being Applied
Maggots Being Removed – Note how much fatter they are after a night of feasting
There’s big news in wound care and you heard it here first. It’s a new study on the cost of chronic non-healing wounds, carried out by the Alliance of Wound Care Stakeholders and published in Value in Health called, “An Economic Evaluation of the Impact, Cost, and Medicare Policy Implications of Chronic Nonhealing Wounds.” I will be talking a lot more about this in future blogs. There is a lot about this study that will surprise you. Access to the paper in its entirety can be found here, so pass it along:
http://www.valueinhealthjournal.com/article/S1098-3015(17)30329-7/pdf

Dr. Fife is a world renowned wound care physician dedicated to improving patient outcomes through quality driven care. Please visit my blog at CarolineFifeMD.com and my Youtube channel at https://www.youtube.com/c/carolinefifemd/videos
The opinions, comments, and content expressed or implied in my statements are solely my own and do not necessarily reflect the position or views of Intellicure or any of the boards on which I serve.