I thought I would wind up 2017 with something that I hope will be a useful tool in 2018. Dr. Jane Armor at the Sinclair School of Nursing, University of Missouri spearheaded the American Lymphedema Framework Project (ALFP). The goal was a systematic review of all the literature pertaining to the treatment of lymphedema. Dr. Wade Farrow and I were tasked with a review of the literature pertaining to wound care in lymphedema associated wounds. We quickly found we could not complete our task as assigned. The reason was that you can’t do a systematic review of the literature if you can’t figure out what the search terms are. Lymphedema associated skin issues are so diverse and referred to by so many different names our first task became the creation of a “taxonomy” for lymphedema-related skin and wound care problems. We did that by first putting together photographic examples of all of these problems, and then asking Dr. Adelaide Hebert, Professor of Dermatology at the University of Texas Health Science Center, Houston, to provide the correct terminology from a dermatological standpoint. We then used those terms for a new literature review, and the result was finally published in Advance in Skin and Wound care in July of 2017 (see 2017; 30: 305-18).
Unfortunately, the ALFP did not fund the publication of this paper “open source.” It’s too bad because I get so many questions related to “what do you call THAT?” in lymphedema patients. So, I am going to reproduce the Rubric for Lymphedema Skin Disorders below, along with some photographs:
Lymphedema Skin Disorders Rubric
Skin Disorders Directly Caused by Lymphedema
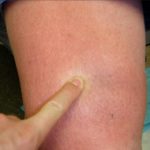
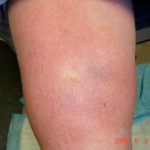
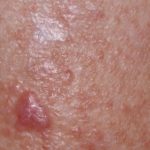
- Lymphedema rubra: the blanchable redness of affected skin due to vasodilation within lymphedematous tissue, often confused with cellulitis [7]. This clinical constellation of findings is not “hot” to the touch and usually resolves with elevation. Lymphedema rubra is felt to represent hyperemia due to proinflammatory changes from the altered protein content of the interstitium and may be similar to the pathology of acute lipodermatosclerosis. See fig. 1a, 1b.
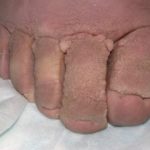
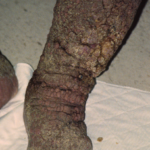
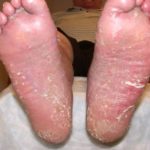
- Skin Fissures: breaks in the epithelium developing between adjacent skin lobules. These slit-like changes in the skin can be superficial or deep, prone to breakdown and wound formation from moisture accumulation and represent common sites for the initial manifestations of fungal infections. See fig. 2.
- Dermal Lichenification: hyperkeratosis, parakeratosis and irregular acanthosis due to overproduction of keratin layers in the skin [8, 9]. The skin is thickened as a function of lymphedema, perhaps exacerbated by chronic scratching and rubbing due to the pruritus of stasis dermatitis.
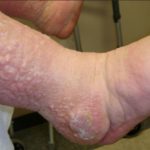
- Papillomas and Fibromas: benign tumors of epithelial, fibrous or connective tissue growing exophytically in finger-like fronds, resulting from the chronic inflammation associated with lymphedema. These tumors can range in size from only a few millimeters to tumors larger than the patient’s digits [9]. Small sandpaper- type papillomas are called fine papillomatosis. See fig. 3.
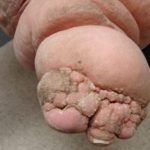
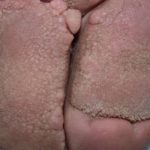
- “Mossy” lesions (e.g. “mossy foot”): extensive fine papillomatosis [8, 10], often with associated lymphorrhea. See fig. 4a and 4b. Internationally, the term “mossy foot” may be reserved for “podoconiosis,” a unique form of lymphedema caused by years of barefoot contact with silicate rich soil. The term “mossy foot” has been used to describe the fine extensive papillomatosis and not necessarily the disease podoconiosis.
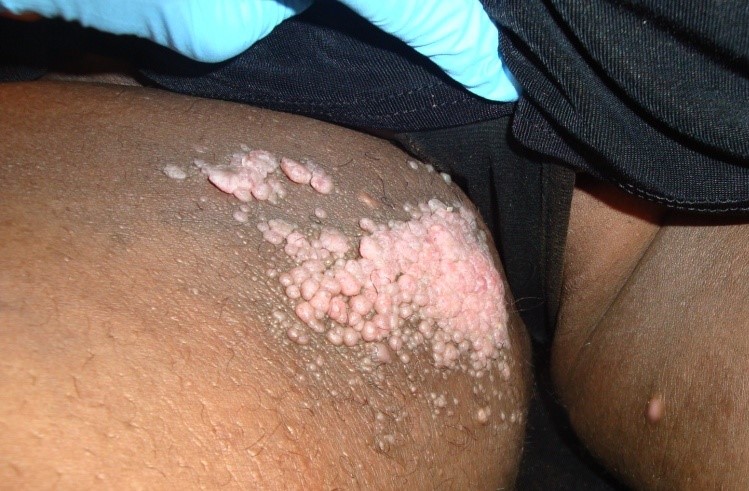
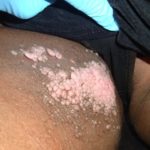
- “Frog’s spawn:” multiple larger papillomas [9-11] that develop due to chronic lymphedema. See fig. 5a and 5b.
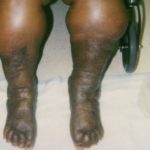
- Dermal Fibrosis: woody changes of the skin [12]. When associated with venous stasis, the legs are often referred to as having an “inverted champagne bottle” shape or a “bowling pin” deformity. See fig. 6.
- Nodular Fibrosis: protruding isolated fibrotic lesions due to chronic inflammatory process of the skin [13, 14]. See fig. 7.
- Lymphangiectasia / Lymphangioma: dilated lymphatic vessels [9, 11].
- Lymphorrhea / Lymphocutaneous Fistula: leakage or weeping of lymph fluid through the skin surface. Drainage can be copious. Lymphatic fluid may transude through a region of the skin [9, 12], or may be caused by a lymphocutaneous fistula (passageway between a lymphatic vessel and the skin).
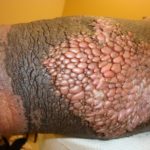
- Elephantiasis Verrucus Nostra: characterized clinically by malodorous hyperkeratosis with generalized lichenification, cobblestoned papules and verrucous changes of the skin. This is often associated with chronic lymphedema that is associated with extreme enlargement of the involved body part. Without intervention, slowly progressive cutaneous changes will result in grotesque enlargement of the affected area [15]. Castellani coined the term “elephantiasis nostra” (meaning “from our region” and not due to filarial disease). Castellani theorized that regardless of subtype, the cause was repetitive streptococcal bacterial invasion causing lymphangitis with subsequent obstruction of lymphatic outflow and the development of elephantiasis. Although striking clinically, histological examination reveals only pseudoepitheliomatous hyperplasia with dilated lymphatic spaces in the dermis, accompanied by chronic inflammation and fibroblast proliferation. [8, 10]. Fig. 8a and 8b
- Massive Localized Lymphedema (MLL): large solitary polyps, solid or papillomatous plaques, pendulous swellings or tumors mimicking sarcoma. These findings are usually associated with obesity and are often mistaken for malignant tumors, hence the term “pseudosarcoma.” A series of 24 patients with MLL reported that the tumors were significantly correlated with history of cellulitis and obesity (p, 0.05) [16]. The mechanism is assumed to be stagnation of proteins and associated water in the interstitium which leads to inflammation and an accumulation of fibroblasts, adipocytes and keratinocytes that transform the initially soft edematous tissue into hard fibrotic tissue with stiff, thick skin. Activated cytokines stimulate the development of redundant tissue. Histologically, all cases exhibited dermal edema, fibroplasia, dilated lymphatic vessels, uniformly distributed stromal cells and varying degrees of papillated epidermal hyperplasia, inflammatory infiltrates, and hyperkeratosis. [9, 11, 16]. See fig. 9, 10.
- Lymphangiosarcoma: a rare malignant tumor which can occur in patients with long-standing lymphedema [17].
- Fig. 1a: Demonstration of lymphedema rubra in patient with Phlebolymphedema.
- Fig. 1b: Demonstration of lymphedema rubra in patient with Phlebolymphedema – Photo taken directly after finger release.
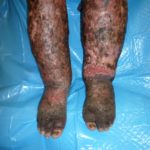
- Fig. 2: Severe elephantiasis of chronic lymphedema of the foot with papillomatosis, lipodematosclerosis, nodular sclerosis, and fibrosis of dermal skin. Note prominent skin fissures.
- Fig. 3: Fibroma
- Fig. 4a: Mossy foot (see area inside box enlarged)
- Fig. 4b: Note fine papilomatosis
- Fig. 5a: “Frog’s eggs” changes in a patient with lymphocutaneous fistula of the groin
- Fig. 5b: “Frog’s eggs” changes on the leg
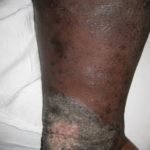
- Fig. 6: Classic Champagne bottle change of Phlebolymphedema (CVI with secondary lymphedema development and woody change dermal fibrosis).
- Fig. 7: Patient with extensive nodular fibrosis changes of advanced phlebolymphedema with lipodermatosclerosis.
- Fig. 8a: Elephantiasis Verrucus Nostra
- Fig. 8b: Elephantiasis Verrucus Nostra (same patients) after months of treatment with lactic acid and hydrocolloid dressings
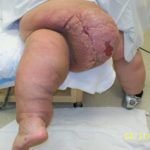
- Fig. 9: Massive Localized Lymphedema (MLL) of the posterior thigh with ulceration
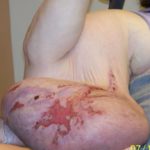
- Fig. 10: Massive localized lymphedema of the upper arm with pressure ulceration
- Fig. 11: Lichen simplex chronicus
- Fig. 12: Fungal infection
- Fig. 13: Lipodermatosclerosis in patient with phlebolymphedema
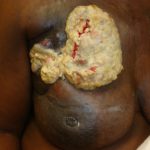
- Fig. 14: Breast cancer patient with autoamputation type ulceration (See fungating breast cancer below if you like this photo better since we discuss fungating tumors). The patient has breast lymphedema
Skin Disorders Indirectly Related to Lymphedema / Obesity
- Folliculitis, lymphangitis, cellulitis [18]
- Dermatitis and eczema [9].
- Lichen simplex chronicus (thickened, leathery, hyperpigmented skin usually caused by recurrent irritation such as the “itch-scratch” cycle) See fig. 11
- Fungal infections [9]. See fig. 12.
- Pressure ulcers from heavy limbs [9] See. Fig.10.
- Limb enlargement and distortion due to fatty deposition (Fig 2)
- Skin disorders associated with diseases causing lymphedema
- Non-healing surgical wounds
- Radiated wounds
- Malignant wounds
- Traumatic wounds
- Venous stasis ulcers and Phlebolymphedema
- Lipodermatosclerosis and stocking erythroderma
Skin and Wound Care in Lymphedema Patients: A Taxonomy, Primer and Literature Review. C Fife, W Farrow, A Hebert, N Armer, J Cormier, J Armer, Advances in Skin and Wound care, 2017; 30: 305-18.

Dr. Fife is a world renowned wound care physician dedicated to improving patient outcomes through quality driven care. Please visit my blog at CarolineFifeMD.com and my Youtube channel at https://www.youtube.com/c/carolinefifemd/videos
The opinions, comments, and content expressed or implied in my statements are solely my own and do not necessarily reflect the position or views of Intellicure or any of the boards on which I serve.




So nice to see terms with actual lics..well written..im a pt, clt just looking for info!
Thank You! I’m an RN and have always wondered what these conditions are called – here they are in 1 spot so I really appreciate this article!!