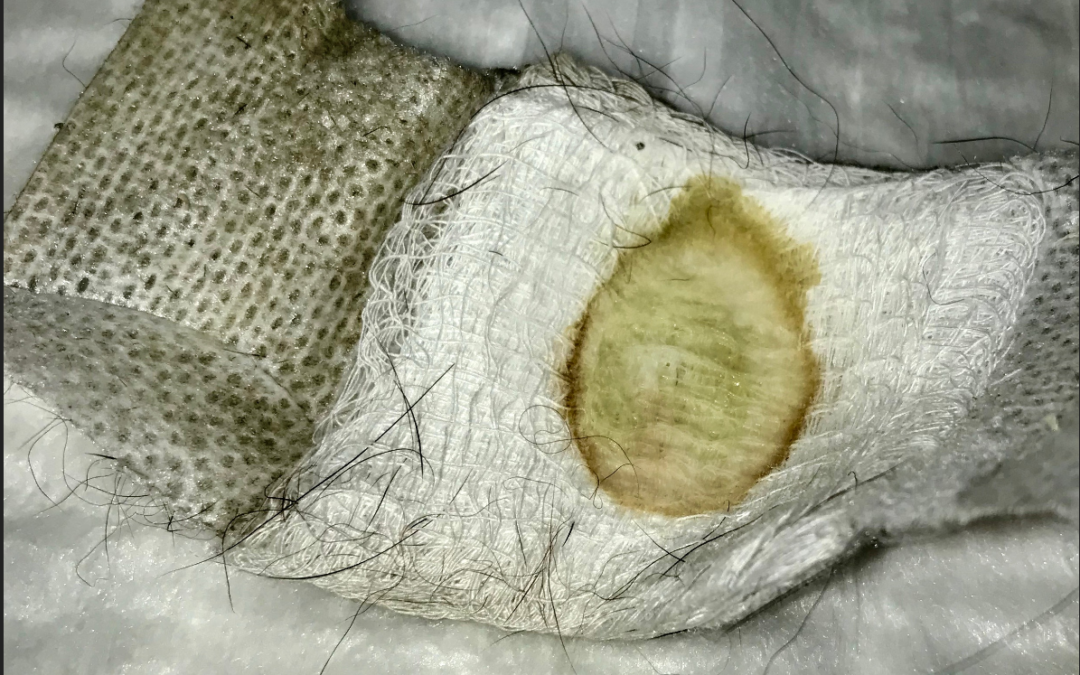
This 34 year old patient is a Type 1 diabetic status post kidney pancreas transplant on life-long immunosuppressive medications who now has a neuropathic foot ulcer. That’s dog hair all over the dressing, which the patient argued was nothing to worry about because the dog hair was not actually INSIDE the wound.
Here is the wound which probes to bone. I got the patient to agree to a Total Contact Cast since it’s clearly necessary to protect this wound

Here are the results of the DNA assay by MicrogenDx.

I am still figuring out how to best use DNA assays, but this one is interesting. I got my microbiology degree from Google in about 15 minutes so I am sure some of you know more about these bacteria than I do, but here’s what I found:
- Porphyromonas cangingivalis is a bacteria found in the periodontal pockets of dogs
- Haemophilus parainfluenzae can be part of the normal flora of the mouth but brain abscess, liver abscess, osteomyelitis, pneumonia, peritonitis, septic arthritis, and bacteremia have been reported to be caused by it.
- H. kunzii is primarily recovered from infected wounds, particularly diabetic foot ulcers with cellulitis
- Anaerococcus lactolyticus is a human pathogen found in chronic wounds that is involved in polymicrobial infections.
- Peptoniphilus harei is part of the normal vaginal and gut microbiota but can be part of polymicrobial infections of diabetic skin and soft tissue, bone, joint and surgical site infections.
- Anaerococcus hydrogenalis is isolated from human feces and vaginal discharge.
On second thought, maybe it’s the dog that needs to worry.

Dr. Fife is a world renowned wound care physician dedicated to improving patient outcomes through quality driven care. Please visit my blog at CarolineFifeMD.com and my Youtube channel at https://www.youtube.com/c/carolinefifemd/videos
The opinions, comments, and content expressed or implied in my statements are solely my own and do not necessarily reflect the position or views of Intellicure or any of the boards on which I serve.



EXACTLY!!! Why we strive to have dressings left on between clinic visits. We have had too many bacterial contaminants that only live in the nether regions of the human body show up in wound cultures. We also do not allow our patients to shower for the very same reason. Not very popular, but does help in reducing cross-contamination.