A very special thanks to Dr. Rafael Rafos, MD for today’s guest post. He sent me this case, and it was so interesting that I asked that he guest blog it for us.


Always trust your instinct! Whenever a wound bed looks “off” or something feels “just not right”, don’t hesitate to biopsy.
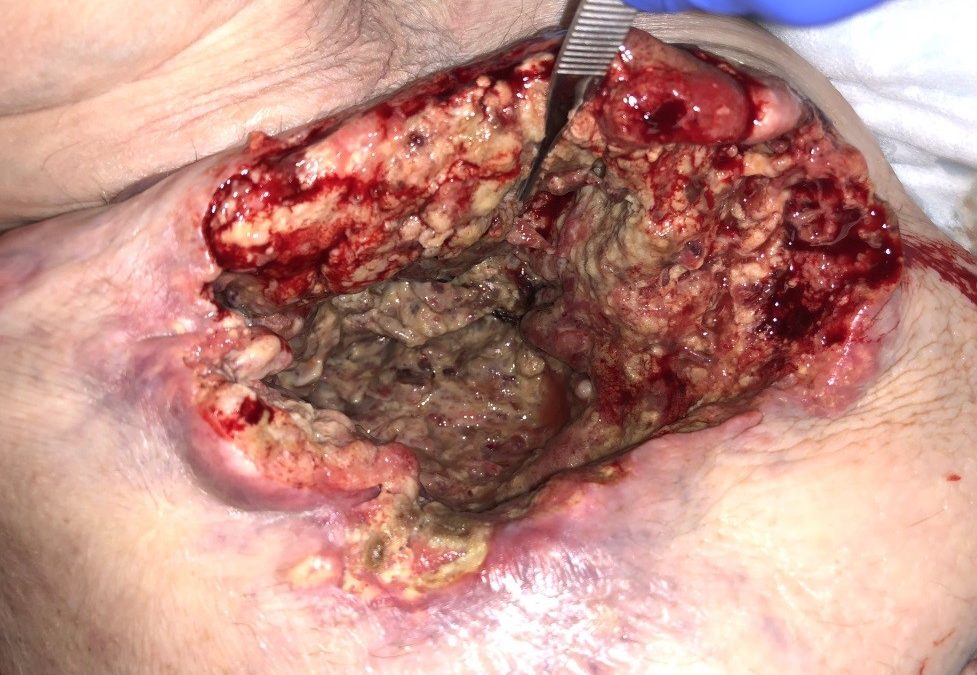
This is the case of a man in his 70’s with history of shoulder arthroplasty with subsequent prosthesis infection and removal due to infected hardware. He subsequently developed chest wall erosion and cellulitis, and was previously treated for Pseudomonas infection with IV antibiotics and NPWT. We were consulted for non-healing wounds.
Something about this wound bed did not seem right. Despite a few weeks of proper wound management, the wound be failed to show any improvement. Furthermore, the wound margins appeared rolled and raised and showed a clear lack of granulation tissue. This should set off your radar!
An excisional biopsy of the wound margins was done…

Suffice it to say, this changed the outlook of the case significantly. After discussing with the family, they were surprisingly appreciative, because we were able to give them a diagnosis and explain why the wound was not healing. Afterwards, they chose hospice and palliative care.

Dr. Fife is a world renowned wound care physician dedicated to improving patient outcomes through quality driven care. Please visit my blog at CarolineFifeMD.com and my Youtube channel at https://www.youtube.com/c/carolinefifemd/videos
The opinions, comments, and content expressed or implied in my statements are solely my own and do not necessarily reflect the position or views of Intellicure or any of the boards on which I serve.