A recent National Academy of Medicine discussion paper reviews the concept of “team-based healthcare” and the way in which it is associated with both improved patient outcomes and clinician well-being.
According to the authors, teamwork must, “enhance the capability of members to work together,” and “contribute to the growth and personal well-being of team members.”
I’m an old-fashioned girl and given to reductivist thinking, so I believe we first have to ensure that team members are competent at their job functions before we concern ourselves with their “personal growth and well-being.” However, physician burnout is at an all-time high and with it the physician suicide rate. I also don’t meet many nurses who say they love their job. And, since I work with an amazing team, I can vouch for the fact that a good healthcare team can achieve clinical goals for the patient and personal goals for the team members when it functions well.
The authors of the discussion paper on team-based healthcare discuss key characteristics of successful team-based care:
- Members share a clear and compelling purpose or goal (I’d call that a mission statement)
- There is a social structure that facilitates teamwork (members must be able to learn, teach, communicate, think together, and achieve shared goals regardless of their individual positions or status outside the team)
- There must be an organization that supports the team concept and function
- There must be trust between the members so that they can admit a mistake, ask a question, offer new data, or try a new skill without fear of embarrassment or punishment
One of the nurses who works occasionally in our wound center is actually the coordinator of the liver clinic down the hall. This evening I asked her advice about a mutual patient and she taught me about the “MELD score” for liver disease. Together we decided that the patient’s worsening edema is probably NOT due to his liver (other than his low albumin), and most likely is a problem for his cardiologist. Thus, two hours later I was having a great conversation with the cardiology Nurse Practitioner to ensure that special attention is given to his edema during the follow up visit about his echo this week. I’m worried about his sleep apnea and possible pulmonary hypertension. The Cardiology NP’s comment about our conversation was, “This is the way care is SUPPOSED to work!”
Teams are hard to build and maintain outside of organizations designed to foster them, but I’ve still managed to create them as well as participate in teams created by others. It’s challenging to get all the agendas to align, including the patient’s. However, there’s no question that when team care is done right, the patient can feel the difference and so can we. I love it when my nurses start a sentence with, “Here’s what I think we ought to do . . .” I am certain we get to a better decision together.
We had a tough day in the clinic today. It started very early with a SCUBA diver who needed an evaluation and an explanation of her unusual case of decompression illness. The next new patient brought a 12-page itemized list of his symptoms. After that I explained (shouted) the nature of venous disease and the rationale for compression bandaging to a 100 year old woman with a good sense of humor and a bright mind but who is almost completely deaf. We diagnosed a case of pyoderma gangrenosum in a C-section that had been missed by other practitioners, and possibly another case of PG one in a pressure ulcer. We managed to keep two fragile patients out of the hospital, and got one very sick lady admitted for observation. I couldn’t do it without the team.
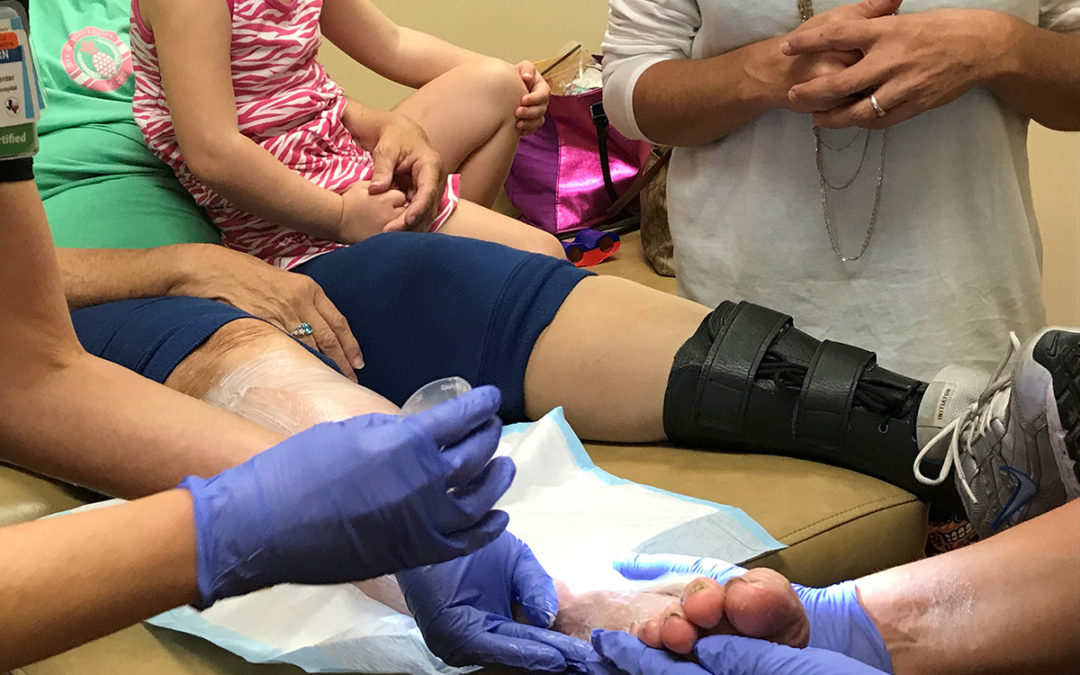
Above is a photo I took of two of my nurses teaming-up to handle one challenging patient who drives from very far away so she has to bring her granddaughter with her (who is sitting on her lap). Her daughter (in the white shirt) performs her interval dressing changes including her compression bandaging, and does a fabulous job. The nurses are reviewing instructions with the daughter while they work.
I know my staff went home weary, and I am so exhausted I keep drifting off to sleep as I type. But I’m not burned out – because I have an awesome team.

Dr. Fife is a world renowned wound care physician dedicated to improving patient outcomes through quality driven care. Please visit my blog at CarolineFifeMD.com and my Youtube channel at https://www.youtube.com/c/carolinefifemd/videos
The opinions, comments, and content expressed or implied in my statements are solely my own and do not necessarily reflect the position or views of Intellicure or any of the boards on which I serve.