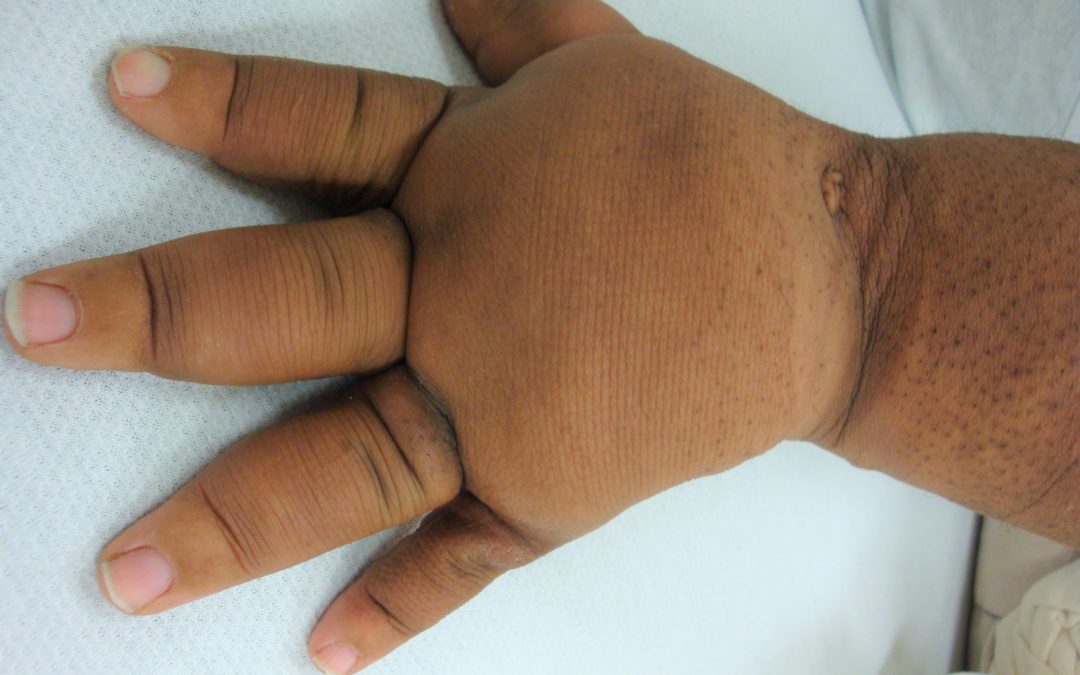
I’ve been thinking a lot about lymphedema due to venous disease vs. other types of lymphedema. I think the differences are worth pondering. We see the impact of venous disease so often that it is a bit like living in a war zone – after a while the abnormal becomes routine. The photo above is the left hand of a 12 year old boy with primary lymphedema. His other hand is normal. He has peau d’orange (“orange peel”) changes of the skin and severe lymphedema, but he doesn’t have any skin breakdown.

The second photo is a woman with lymphedema of the hand after treatment for breast cancer.

…and here is an image of her lymphatics taken with near infra-red imaging of indocyanine green (using Dr. Eva Sevick’s “NIRF” imaging). You can see that there is retrograde flow of the lymphatics toward the fingers, and she even has a lymphocutaneous fistula of the palm. This cancer survivor has a normal appearing right hand, but it’s possible that she had a predisposition for the development of lymphedema as a result of genetic/anatomical factors based on the fact that her lymphatics “flow the wrong direction”. Despite the fact she has a small fistula in her palm draining lymphatic fluid (which she perceived as a very sweaty hand), she doesn’t have any obvious open ulcerations.

The patient above is a man with lymphedema of the hand after a venous occlusion. You can see that he has changes consistent with venous stasis of the hand including hemosiderin deposits. The open ulcers on the fingers are actually venous stasis ulcers which are rather rare in the upper extremity.
The first two patients have lymphedema which originated from lymphatic disease/occlusion (e.g. born with diseased lymphatics or damaged due to cancer treatment). In contrast, patient #3 had a venous occlusion which led to lymphedema. Both primary and secondary lymphedema are inflammatory states that lead to tissue hypertrophy which is why both the 12 year old boy and the cancer survivor appear to have a “fat hand.” The hand really does have extra fat on it as a result of this pro-inflammatory fluid. Lymphedema patients can also develop profound skin changes. We attempted to create a taxonomy for the skin changes associated with lymphedema as part of the “Lymphedema Framework.” Here’s a link to the information.
The fascinating question is, “Why does the patient with the venous occlusion have painful, open ulcers when the other patients don’t?” We take that for granted in the lower extremity, but think about it anew in the upper extremity. Have you asked yourself why some patients with lymphedema have profound skin changes and others do not, and that lymphedema in the setting of venous occlusion is so much more likely to lead to ulceration than lymphatic occlusion in the absence of venous disease?
Direct evidence of lymphatic function improvement after advanced pneumatic compression device treatment of lymphedema. Kristen E. Adams, John C. Rasmussen, Chinmay Darne, I-Chih Tan,1 Melissa B. Aldrich, Milton V. Marshall, Caroline E. Fife, Erik A. Maus, Latisha A. Smith, Renie Guilloid, Sunday Hoy, and Eva M. Sevick-Muraca. 2 August 2010 / Vol. 1, No. 1 / BIOMEDICAL OPTICS EXPRESS 114

Dr. Fife is a world renowned wound care physician dedicated to improving patient outcomes through quality driven care. Please visit my blog at CarolineFifeMD.com and my Youtube channel at https://www.youtube.com/c/carolinefifemd/videos
The opinions, comments, and content expressed or implied in my statements are solely my own and do not necessarily reflect the position or views of Intellicure or any of the boards on which I serve.