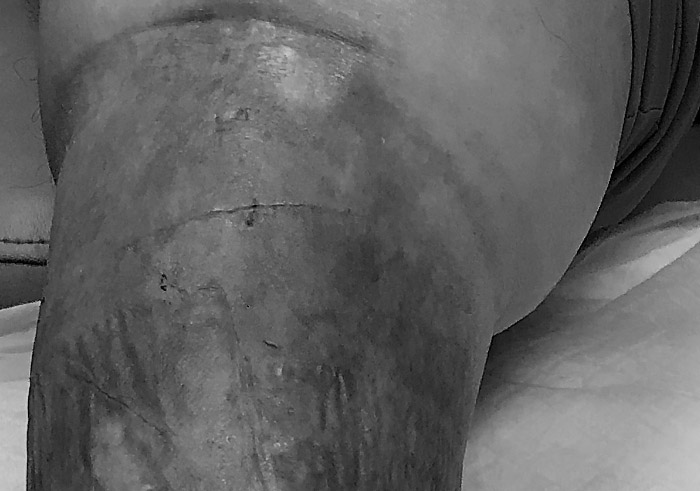
This patient is in is 50’s (younger than I am). He has hypertension, liver cirrhosis, type 2 diabetes, and sleep apnea (he’s a chair sleeper). He’s still obese 3 years after a gastric sleeve operation. He’s chronically fluid overloaded with pitting edema to his groin. He normally doesn’t take his diuretics because they make him have to urinate constantly, and that’s a problem since he goes camping a lot.
It’s true, he does have venous insufficiency with lower extremity lymphedema. However, he first came to see us after bilateral knee replacements when the compression stockings in which he was placed pushed the edema up to his already swollen knees so that the surgical incisions began to weep.

He’s now been followed at the wound center for 7 months, which is at about the national average of 7.5 months based on US Wound Registry data. The reason he has been seeing us so long is that as soon as we get one wound closed, another occurs. That’s because his skin essentially splits apart due to the edema of his legs whenever we try to transition him out of his compression wraps to one of the compression garments. Thus, while it’s true that he has venous insufficiency, it’s also true that these problems are really wounds due to tears in the skin. However, they will probably get coded as venous ulcers in order to ensure he can get clean and operational compression garments (e.g. Farrow wraps, Juzo wraps, Circiad Juxtalight, etc.)
What will happen to him under an “episode of care” model of wound care? When did his wound care episode begin? When does it end?

Dr. Fife is a world renowned wound care physician dedicated to improving patient outcomes through quality driven care. Please visit my blog at CarolineFifeMD.com and my Youtube channel at https://www.youtube.com/c/carolinefifemd/videos
The opinions, comments, and content expressed or implied in my statements are solely my own and do not necessarily reflect the position or views of Intellicure or any of the boards on which I serve.