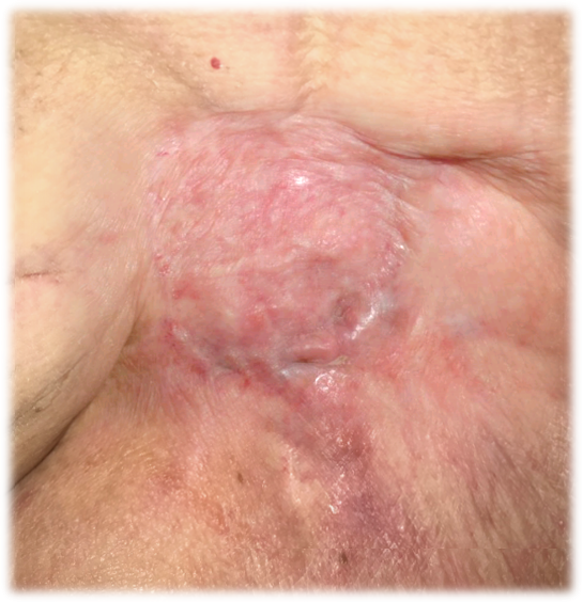
I’ve got a lot of patients who have had very targeted local radiation. Some of them got radiation years ago for really questionable reasons, the others for only recently. The non-healing wounds present in the irradiated field can be small but really persistent. The problem may not meet criteria for hyperbaric oxygen therapy, particularly given the current HBOT audit climate. Their healing rate (if it’s happening at all) is at a glacial pace. I decided to try the OxyBand for these chronic ulcers in an irradiated field. Check out these photos of a patient who had a sarcoma of the sacrum leaving him with a small but persistent wound that had been a nuisance for an entire year if you count the time right after the flap and graft, radiation, etc.
The OxyBand got high marks for patient satisfaction in my informal survey, which brings up another sore spot of my own. The US Wound Registry footed the bill to license a European wound-related Quality of Life (w-QoL) assessment tool, and we developed it into a patient reported quality measure that could be used for credit under the Merit Based Incentive Payment System (MIPS). The USWR collected wound related quality of life data from 400 patients using tablets that transmitted the w-QoL data directly to the USWR. We couldn’t get any monetary support for the project, so we just did it. Unfortunately, no physicians reported Wound Quality of Life as a quality measure (it’s time consuming and there’s no good argument for doing it, regardless of how much everyone SAYS they think it matters.) CMS rejected the unused quality measure after a couple of years. Dr. Marissa Carter was kind enough to pick through the w-QOL data to help us look for some useful observations in relation to wound outcome. When the bright day dawns that we decide we really do care about this and “bake in” some reward for optimizing the patient experience (or conclusively tie it to reduced cost), the USWR knows how to do it. We can put it on tablets and transmit the data to the registry. Until then, I’ve got a big eye-roll emoji for anyone pontificating that we should collect quality of life data.
Back to the patient above. The wound closed 11 weeks after OxyBand treatments began. Check out the results below:
The patient emailed me the following:
“Real improvement was observed with regular use of Oxyband (I had gotten a sample for them to try because I was a bit unsure about the whole thing and their response was to ask for more.) The extended wear aspect of the bandage was convenient. If the Oxyband started to fray at the edges, you could easily reinforce with tape. We are very grateful that we tried this product and we are thankful that you brought it to our attention. With you taking a chance and thinking outside the box we are where we are today. Thank you so very much!”
(And by way of disclosure, I have no financial relationship with OxyBand, but they have generously provided product samples for these patients.)

Dr. Fife is a world renowned wound care physician dedicated to improving patient outcomes through quality driven care. Please visit my blog at CarolineFifeMD.com and my Youtube channel at https://www.youtube.com/c/carolinefifemd/videos
The opinions, comments, and content expressed or implied in my statements are solely my own and do not necessarily reflect the position or views of Intellicure or any of the boards on which I serve.