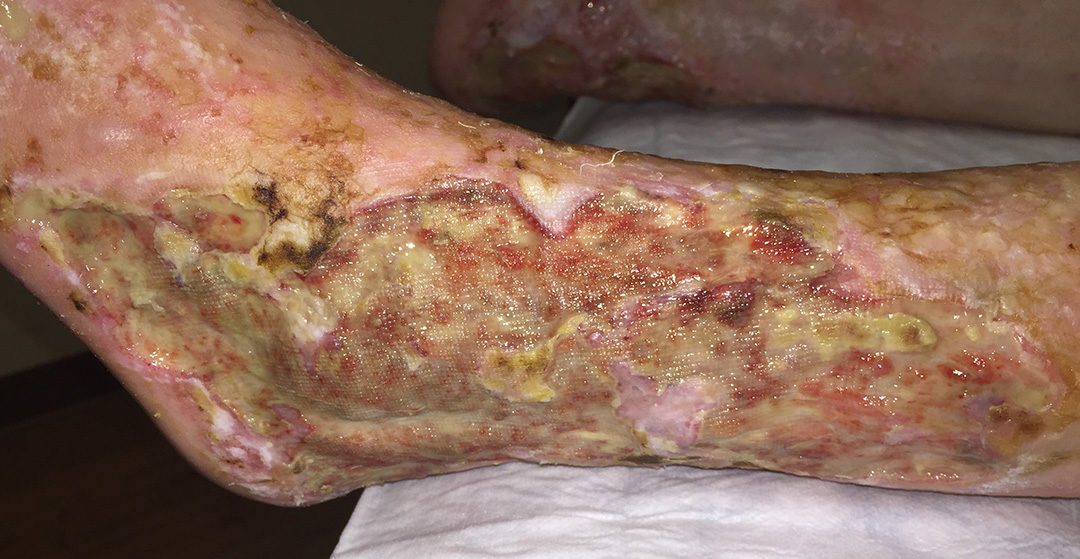
One of the things that makes wound care fascinating is that you can work your way through the Merck manual of rare diseases in a few months. I walked into see a new patient who had some of the worst leg ulcers I have ever seen (see above). He was a diabetic on dialysis and looked sick, but he had a tan. The first thing I said was, “Do you go fishing a lot, or what?” He told me that he never went outside. Nevertheless, he appeared very tan and had dark freckles everywhere:

Then I noticed his spoon nails:

What I thought was “Yikes, I remember this was a board question but I can’t remember the answer!” What I said was, “I’ll be right back.” I am uncomfortable using Google to figure out what is wrong with a patient on their very first visit. I get more comfortable about it after I get to know them since I have to do it a lot . . . You probably remembered this answer to this board question and didn’t have to go look it up – the answer is hemochromatosis. I can talk more about his case some other time, because it’s fascinating. His serum ferritin level was over 2,000 (normal range 24-300 µg/L). His ulcers were huge and drained copiously, but I noticed was that the drainage was GREY. I suddenly realized, he was draining iron:

That got me thinking. I stumbled on an article more than a decade old, published in the Journal of the Royal Society of Medicine, in which Paolo Zamboni suggested what he called, “The Big idea of iron-dependent inflammation.” He points out that with the demise of the “fibrin cuff” theory of inflammation in venous disease, some investigators have focused on the role of iron accumulation in the chronic inflammation of chronic venous disease. Everyone is familiar with the hemosiderin deposits of venous disease – the brown discoloration caused by the deposition of iron as red cells are degraded by interstitial macrophages. It is almost universally present at least in the peri-wound of a venous ulcer. In fact, if you don’t see some hemosiderin, you should question your diagnosis. I didn’t know that hemosiderin has even been demonstrated in the urine of patients affected by chronic venous disease (CVD). He postulated that the white blood-cell migration in CVD patients might actually be a response to underlying inflammation caused by the interstitial iron. The thing that worried me in this patient, who had been cared for at another wound center for 10 years without anyone noticing his apparent spray-tan, was the possibility that his renal failure and his unusual ulcerations could have been caused by iron overload, and perhaps prevented if diagnosed earlier.
Ever since this dramatic case, I’ve been noticing the same gray drainage in some patients with really hard to heal venous ulcers. The patient in this picture has had every venous procedure possible:

His ulcers got dramatically better after I got him on aspirin. However, it’s impossible to keep him healed, and he is the most compliant patient ever with regard to compression. You can see the iron that has separated out in his bandages.
This week I noticed iron in the bandages of a patient with lymphedema and venous stasis who has a plantar foot ulcer. What’s interesting about his case is that he doesn’t have hemosiderin around the plantar wound (it’s abundant on his leg). Nevertheless, it’s present in the exudate coming out of the bottom of his foot, which means it’s not exactly a local phenomenon – but that’s is present in his serum.

What’s interesting about this last case is that the iron is probably present in his lymphatic fluid (which seems to be what drains out of his foot). And that’s a really interesting thing to ponder in a man with severe lymphedema.

Has anyone else got an Ironman?

Dr. Fife is a world renowned wound care physician dedicated to improving patient outcomes through quality driven care. Please visit my blog at CarolineFifeMD.com and my Youtube channel at https://www.youtube.com/c/carolinefifemd/videos
The opinions, comments, and content expressed or implied in my statements are solely my own and do not necessarily reflect the position or views of Intellicure or any of the boards on which I serve.



We have many Ironmen and women! Is Aspirin the only treatment?