As any wound care practitioner knows, you can work your way through the Merck Manual of Rare Diseases every year because wounds are a SYMPTOM of disease. If there’s a rare condition, it will probably end up in the wound center. The question is whether we recognize it. I missed the fact this sweet lady has Ehlers-Danlos syndrome (EDS). EDS is a group of related disorders caused by different genetic defects in collagen. Most of us remember this condition vaguely from medical school textbooks because, thanks to their extreme flexibility, it is the condition which allowed circus performers of yesterday to contort their body to an extreme degree.
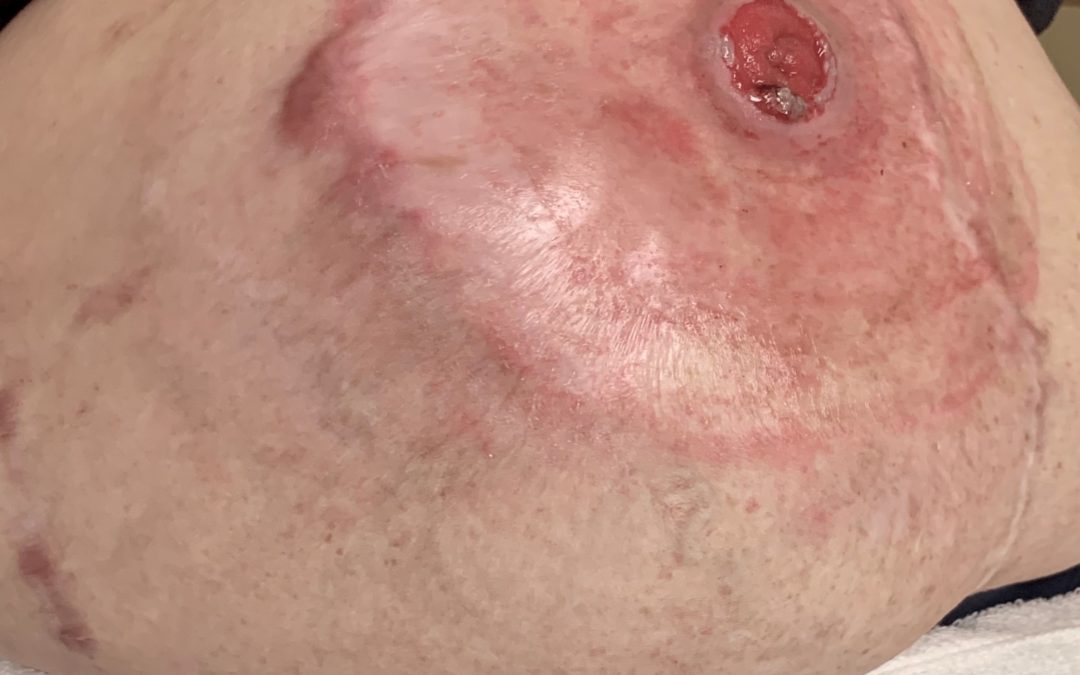
My patient came to the wound center because of complications after abdominal surgery. She had undergone multiple abdominal operations and things always seemed to “fall apart.” Her ostomy kept having to be redone, and she had a massive abdominal hernia (see photo). Whenever a patient’s story is complicated, and you think to yourself, “WHY do they seem to have such bad luck?” then maybe we are missing something. And I was!
Reported estimates for the incidence of all EDS types range from 1/ 2,500 to 1/5,000 births. There are 13 subtypes of EDS each of which has specific clinical criteria, but the primary symptoms are joint hypermobility, skin hyperextensibility, and tissue fragility- which is of course why they have wound healing problems. There is a lot of symptom overlap with other connective tissue disorders so that can confuse the diagnosis. For example, she said her mother had rheumatoid arthritis – but I bet she didn’t. She probably had EDS. Classical EDS follows an autosomal dominant in heritance pattern, but some variants are recessive.
Hints about EDS include paper-like (papyraceous) scars which are discolored and stretch with time (see photos of her scars), frequent joint dislocation and degenerative joint disease which can be associated with chronic pain. Bowel disorders are common including functional dyspepsia (indigestion), irritable bowel syndrome and bowel rupture. They have autonomic nervous system issues and may experience orthostatic hypotension. The more serious complications of some subtypes are cardiac valvular problems (especially the mitral/bicuspid valve) which can lead to congestive heart failure, arterio-venous malformations and dilatation of the aorta with an increased risk of aortic dissection.
My patient likely has the Dermatosparaxis type (dEDS). Manifestations include short stature and short fingers, loose skin (see left photo below), and blue-tinged sclera (see right photo below). A major and common complication of dEDS is herniation after abdominal surgery, in part due to the lengthy wound-healing process (which of course she had). EDS patients are predisposed to wound healing problems. Surgical wounds require extra sutures and should be left in longer. Wound edges should be carefully approximated. Ascorbic acid (Vitamin C) may be recommended to help reduce easy bruising from vessel fragility.

I missed her skin hyperextensibility, parchment paper scars (see below) and faintly blue sclera, but in retrospect, it’s so obvious. I wonder how many others I have missed? She said she wanted me to post these photos because one of you reading this blog has a chronic wound patient with undiagnosed EDS. I hope you will pass this one on.

More Information:

Dr. Fife is a world renowned wound care physician dedicated to improving patient outcomes through quality driven care. Please visit my blog at CarolineFifeMD.com and my Youtube channel at https://www.youtube.com/c/carolinefifemd/videos
The opinions, comments, and content expressed or implied in my statements are solely my own and do not necessarily reflect the position or views of Intellicure or any of the boards on which I serve.



Thank you for sharing. Yes, I will pass it along. Thank you for this website, you’re articles are amazing!
Dr – I almost teared up reading this. You have NO IDEA our frustration with the lack of catching this syndrome. I have VERY noticeable signs and symptoms that after I was diagnosed (by a NP in the PARKING LOT of where I worked FOR A CARDIOLOGIST) as an ultrasound tech and I had been stationed WITH a medical unit in the army AND stationed and living among a BUNCH of Drs and surgeons and EVERYONE missing my vascular and hypermobile EDS.
My mom was killed in car accident we were in with almost a TAP as a truck tapped into us in the snow as we were spinning in place – aortic dissection killed instantly (she was 43, I was 15)
My shoulder dislocated and “blood spots on my brain” and collarbone broken …..
I couldn’t ever RUN in the military even though I did Navy AND Army….because I have POTS. They just NEVER took my hr STANDING so missed it every time and I was treated VERY poorly by my superiors (ma’am we would call what they called me…. a “shitbag”
I’ve also had something that has only happened 62 times in written history since 1901. (If you get this pls ask me about it – it’s MORE than fascinating)
I have had back surgery at 33 and 11 yrs ago I fell off a bike and, we ALLLL thought, it rebusted my disk. I went through hydro addition, multiple half-assed attempts at suicide (if I had not been raised believing you go to Hell if you kill yourself which I strongly believe) I would have offed myself a month into it….
The sciatic pain was SOOOO encompassing and severe that I just couldn’t EVER eat, sleep or do ANYTHING to just make my life…..live able….
I just wanted to DIE…EVERY second of EVERY day for the next NINE YEARS. No exaggeration….NINE YEARS….
At the end of those nine years I had been JUST recently diagnosed, I was 96lbs at 6’1, I was almost completely invalid (I lived with my older coworker and he bathed and dressed me and took me to hospital and tried to help me as MUCH as possible at work). I had gone cold turkey at the pleading of my gpa 5 YEARS before, so only took occasional ibuprofen….
Ma’am – I was in MORE pain for NINE YEARS that I have EVER seen ANYONE in in my whole life…..other than acute SEVERE injury…
So, one day I’m using my walker and taking a pt back to prep for vein ablation and this PATIENT said to me “that’s not your back, that’s your hip!!!!”
I tear up as I recount this story because He LITERALLY saved my life. I WOULD have killed myself SOON. I had access to a gun. I just didn’t want David or my dogs to find me.
I had ALREADY been seeing a chiropractor that put me into SEVERE muscle spasm when they cracked me using my hip rotated….
WHY?!?! BECAUSE I HAD BEEN WALKING ON A DISLOCATED HIP FOR NINE YEARS!!!!!
Called a DIFFERENT chiro and he agreed to see me…at this point I wasn’t even SURE it was my hip but I’d do anything at this point:
Went THAT evening to him and without even taking a X-ray or taking more money, he put me on a drop table and dropped my hip back into place for the first time in NINE YEARS!
The LACK of pain was SO overwhelming I just laid there and SOBBED….
I slept that night for the first time….
I woke up the next morning and got my rail-thin body into the shower and as I leaned back to wet my hair……Thunk…..
They pain came SCREAMING back twice as bad as before because my hip was PISSED that I had DARED try to fix it…..so I SOBBED in despair this time. Then I paused to ????, what if I could REPLICATE the movement? So I hobbled Out to my bed, situated my leg ???? like that and SLAMMED my knee down on the bed many times until …..thunk…..I DID IT!!!!! So I taught myself how to do that standing up at work and put it back into place 50 times a week at LEAST……
Then I joined the gym. After nine years I had elbow brace, two knee braces, a brace for my back that didn’t work because I was SO thin, and both ankles and sometimes some KT tape around my fingers.
As the months went by I gained 60lbs, ate very healthy, and took those braces off one-by-one (I only wear my elbow brace rarely)
That was 2 1/2 Years ago. I now at 45 yrs old, sleep in a recliner so have no love life. Take Kratom for pain (WONDER WONDER WONDER leaf) (I stopped even taking Xanax for my POTS) and I mow my lawn every week and instruct ultrasound with no issues other than my eyesight and fatigue……
My face stretches out like Joker from Batman if I slightly pull on it and I have the blue sclera and Karatoconus BAD. My teeth have no gums left on it so have NO idea why haven’t lost more since…..
I’m starting to struggle with Sjogrens (my grandma lived to 93 with having no saliva or tears for the last 29yrs of her life)
As a cruel twist of fate I’m getting that from the OTHER side of my family. I THINK ????……sjogrens can be seen with EDS also….
I have no (praise Jesus) aneurysms at this time and only mild MVP of the heart….
I KNOW this was REALLY long but I wanted to reach out so we can work TOGETHER on education….
You know ????
If you were to advert yourself as someone that will see EDS patients you’ll have ppl that will fly in from across the country just so someone will tell them “you’re NOT crazy” even though they may look perfectly normal…. and in MY case I do NOT look 45 (I got asked out by a 32 yr old today woohoo ???? lol)
PLEASE contact me if you’d like to see pics or learn about that VERY RARE thing that happened to me (you could even, I’m sure, do a case study and get it published)
THANK YOU so much from ALL OF US!!!!
I’ll leave you with this EDS motto.
“When you hear hoofbeats, think Zebras”
This is our mascot also, the zebra.
God Bless to you and yours
Mary Baker, RVT
I am going to my dermatologist today this is so me!! Thank you for writing this.
Thank you for posting. I have Eds and saw a wound doctor who knew nothing about Eds along with my surgeon who knows very little. I’m still struggling to receive treatment to close my wound after infection and opening of incision.
Hello, Caroline! This is Christie Funderburk 🙂 I just wanted to thank you so much for your article on EDS because I “just happened” to click on your article because my daughter, Grace, is having a complicated hip surgery this week. She has all the symptoms of hypermobile EDS. And now, I can mention to the surgeon, that he might want to consider using more sutures than normal, along with giving her extra time to heal. I’m so grateful for your insight, pictures, and willingness to share your recommendations here. I’m so glad that I saw your article prior to Grace’s surgery! Thank you so much!
I’m at a loss at the cruelty the Medical Community usually ignorant of this condition consistently demonstrates-a condition that isn’t that rare in a ‘shrinking’ and evolving international world culturally. One in 5000 is not so unusual. It is carried by dominant genetics by only one parent To refuse to educate themselves and responsible comprehensive medical providers in light of the complications EDS can burden patients with is unconscionable.
I have gone into consultation situations where unless educated I would have been entirely dismissed- in others I am myself a doctor provider and have been intellectually bullied and humiliated by providers who either did not feel EDS was ‘real’ or in spite of being the only specialty referral available were uninformed about EDS so unequipped to be offering care.
I often rationalize am in SW USA and not in an area where the population has a high probability of having EDS so try and understand. But when EDS has to be considered to ensure the optimal outcome of medical care I am usually very
However very recently my Breast CA Team at UNM were very different. I was relieved not only to have to explain it, Dr. Thompson (before retiring) in Nuclear Medicine was aware how complicated it could get from my skin and collagen abnormalities with radiation treatments. My oncologist Dr. Neumanitis was excellent. She was both comprehensive and conservative in her cautious care in the removal and subsequent chemo treatment. Unfortunately they didn’t have information whether EDS predisposed me to CA in any specific way or if needed to treat more carefully. I wanted to know if it would more likely metastasize due to abnormalities EDS patients have but no one knew.
My Surgeon, Dr. Prebakarian, is conservative and very thorough. She was understood my caution 2 months ago. Not ever entirely recovering – Im exhausted nauseous; autonomic dysfunction and sweating- she made sure I got a Breast MRI. EDS complications aside, we found more large tumors in the liver. We are hoping the medical community can share any information about Cancer treatment complications of EDS. The liver biopsy 2 days ago will probably lead to care decisions that we may assistance making.
Thank you for being an available forum
Susan
Bravo, thank you for your honesty and transparency as a medical professional.