Pyoderma Gangrenosum (PG) is one of the most painful wounds we see each year. It is called a “rare” disorder with an estimated incidence of 3 to 10 cases per million people per year.(1) That would mean there are about 20 new cases of PG in Houston, Texas each year. The problem is that I see at least 8 a year in my little clinic alone, so I think it might be more accurate to say that PG is rarely diagnosed.
PG is characterized histopathologically by the accumulation of neutrophils in the skin. Unfortunately, once it’s been active for several months, biopsies may not be very useful and you have to rely on the history. I happen to enjoy taking a careful wound history.
The most common presentation of PG is the rapid development of one or more painful ulcers, sometimes with what appears to be purulent discharge, and undermined, irregular borders, usually on sites of normal or traumatized skin. It is also common for patients to have some underlying systemic inflammatory condition (e.g. rheumatoid arthritis, psoriatic arthritis, inflammatory bowel disease, etc.). So, PG should be high on the differential diagnosis list of any patient with a history of an inflammatory condition who has developed an agonizingly painful ulceration after minor trauma, or at the site of a surgical incision. In the past 2 years I have seen three cases of PG after cosmetic breast surgery (e.g. breast reductions). Take a good history for bowel disease. I once saw a young woman with obvious PG lesions on her leg. I asked her if she ever had blood in her stools or bloody diarrhea after she ate and she said, “Doesn’t everyone?” She had undiagnosed IBD.
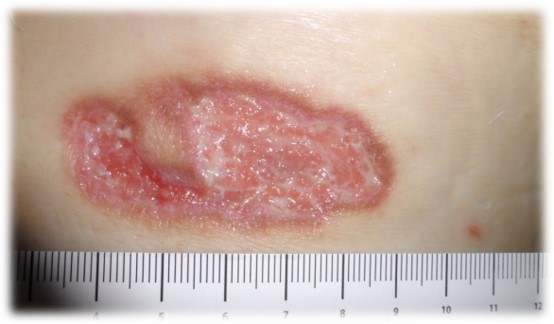
I think I will show a few photos just to focus on the many faces of PG, with just a little info about the patients that tipped me off. In a few cases I had patients grind up 1 mg Prednisone tablets and sprinkle it in the wound – but that’s for smoldering cases. The acute ones need oral Prednisone, and I usually start at 60 mg per day.
https://rarediseases.org/rare-diseases/pyoderma-gangrenosum/

Dr. Fife is a world renowned wound care physician dedicated to improving patient outcomes through quality driven care. Please visit my blog at CarolineFifeMD.com and my Youtube channel at https://www.youtube.com/c/carolinefifemd/videos
The opinions, comments, and content expressed or implied in my statements are solely my own and do not necessarily reflect the position or views of Intellicure or any of the boards on which I serve.



I have this. Thank you for all you are doing.
I believe I have this and have so far been untreated as they’re trying to eliminate all other possibilities. I’m back in hospital tomorrow but need second biopsy results back to eliminate fungal infection so they will go ahead with steroids. It’s been a 9 month nightmare 😭