Even when it’s not possible to fix what is physically wrong with patients, we can often improve their mental well-being. Sometimes the most important thing we can dispense is what I would call “grace.” I worry that it’s gotten harder to find healthcare professionals who provide that kind of caring, and most patients are grateful when they find it. Unfortunately, there are patients who negatively impact the mental well-being of the healthcare providers. Some are dangerous. A few months ago, we were treating a man who excused his regular fits of rage and belligerence as the aftermath of a traumatic brain injury, behaviors over which he claimed to have no control. I suspected Mr. Volatile’s behavior was indeed under his control but decided to give him the benefit of doubt, at least for a while. Healthcare providers cannot expect to avoid risk in our professional lives, but we can mitigate it. It is a sad fact that 75% of workplace violence events occur in healthcare facilities (see resources below). I needed a responsible plan of action given that the entire clinic staff (front desk, nurses, all 3 doctors and the hyperbaric technician) are petite females who don’t meet the weight requirement to donate blood. I wrote up a patient contract about acceptable behavior — which he refused to sign. We held a staff meeting to review the “shelter in place” action plan (e.g. nurses go into the exam rooms with patients, block the door, call security, etc.). And, I arranged for hospital security to be visibly present in the clinic whenever Mr. Volatile had an appointment.
Meanwhile, my poor husband was losing the battle with dementia. He had been a kind and even-tempered man, which is how I will remember him. When an impulsive guy with an anger management problem took possession of my husband’s body, it was easy for me to pretend I was looking after a stranger while my husband was away. He had also been the responsible one with money — until he started donating my entire monthly salary to charity. Since many charities sell the contact information of their donors to other charities, the postman had begun delivering our daily mail in a plastic bin, filled entirely with solicitations. Before I realized what had happened, he had donated to most of them, particularly if it involved a hungry child or a mistreated animal. (FYI, there is a charity called “Save the Donkeys” and yes, the donkeys are cute.) That’s why it was sadly ironic when he got it into his head that I hadn’t paid the credit card bill. At 2 AM he was standing in his study, yelling that I was going to ruin his credit score. Purple in the face, he concluded his rant by shouting, “This is ALL YOUR FAULT.” Since angry, demented people are not influenced by fact-based arguments, redirection is your best bet. I smiled and acknowledged that my ruining his credit score had always been a very legitimate possibility and the fact we’d had a superior credit rating for 30 years was entirely due to his reliability. I promised to have the accountant call him first thing in the morning. Thus satisfied, he began lamenting the fact it was too late for a chocolate dip cone from Dairy Queen.
Six hours later, I was in clinic with Mr. Volatile. It was Monday morning and the previous Friday (when I wasn’t there), he had yelled at the staff. I was weary so my body was relaxed, my hands in my coat pockets, and I started a casual conversation with, “Remember our discussion regarding what behavior was acceptable with the staff…?” Now, it IS my fault that I hadn’t checked to see if hospital security had arrived before I went in the exam room, but in my defense, I was tired. In a spectacular show of speed and agility, Mr. Volatile lunged at me, stopping only inches from my face. He was in extremely good physical shape and since I am only just a bit over 5 feet tall, the intimidation impact was impressive. Several minutes of shouting ensued, at the end of which his face turned purple and he bellowed, “THIS IS ALL YOUR FAULT!” The talk track running through my head was, “I seriously cannot believe that in less than 24 hours, two different enraged men have said that exact same thing to me. What are the odds of that?” I mean, I am responsible for a lot of things, but your being crazy isn’t one of them. The situation was so ridiculous that I couldn’t help myself — I laughed.
And then an astounding thing happened. When I genuinely laughed in response to his in-your-face screaming, he completely changed his tactics. He sat down in a chair and started trying to negotiate with me. That of course, confirmed my suspicions that his behavior was entirely under his control. My brain started to function a little better and I surreptitiously removed my glasses in case I took a face punch. Glasses frames are darn expensive, and I was short of cash on account of saving the donkeys. In truth, by then there was little chance he’d take a swing at me because he’d given me control of the encounter when he sat down. I told him that since he’d just threatened me, I wasn’t going to negotiate. I took hold of his arm and propelled him out of the clinic to the main elevators and into the arms of two Security guards who had finally arrived. In a few hours a judge had issued a restraining order and that was the end of the problem, except for the time it took to reassure several wide-eyed patients who were huddled in the other exam rooms.
I am quite sure that if I’d hadn’t had a practice drill 6 hours earlier with the angry man who inhabited my husband’s body, my reaction to Mr. Volatile would have been exactly what he intended and usually achieved — fear. It’s also likely that the real explanation for this happy ending was divine protection, and I don’t say that glibly. I really mean it. It was, however, a good demonstration of how responding in a completely unexpected way can disarm an aggressor, at least long enough for you to gain some control. It also demonstrates how even a little training enables people to respond better in a crisis, that God’s ways are not just mysterious – they are downright peculiar, and that if someone chooses not to accept grace, it is not my fault.
Here are some things to remember about safety in the healthcare setting:
- Patients are the largest source of violence in healthcare settings.
- The vast majority of workplace violence occurs in healthcare settings. According to the Occupational Safety and Health Administration (OSHA), approximately 75% of workplace assaults occur in healthcare and social service settings.
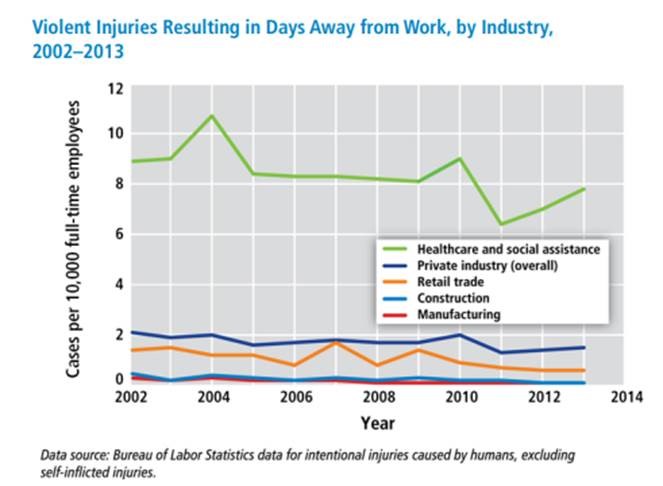
- Healthcare workers are 4 times more likely to be victimized than workers in private industry.
- Over a 12 month period, 21% of registered nurses and nursing students reported being physically assaulted and over 50% were verbally abused (2014 American Nurses Association’s Health Risk Appraisal survey of 3,765 registered nurses and nursing students).
Workplace Violence Prevention Resources:
- Sentinel Events, Joint Commission
- Workplace Violence in Healthcare: OSHA
- OSHA’s Guidelines for Preventing Workplace Violence for Healthcare and Social Service Workers describe the five components of an effective workplace violence prevention program, with extensive examples.
- Preventing Workplace Violence: A Road Map for Healthcare Facilities expands on OSHA’s guidelines by presenting case studies and successful strategies from a variety of healthcare facilities.
- Workplace Violence Prevention and Related Goals: The Big Picture explains how you can achieve synergies between workplace violence prevention, broader safety and health objectives, accreditation, and a “culture of safety.”

Dr. Fife is a world renowned wound care physician dedicated to improving patient outcomes through quality driven care. Please visit my blog at CarolineFifeMD.com and my Youtube channel at https://www.youtube.com/c/carolinefifemd/videos
The opinions, comments, and content expressed or implied in my statements are solely my own and do not necessarily reflect the position or views of Intellicure or any of the boards on which I serve.




That was excellent!
I wasn’t sure to laugh or cry over this. TEI sad situations and your humor really softened it. Scary situation withTh Mr volatile that could have had a different ending. I didn’t know the rate of violence in the healthcare setting – 75%. Wow. Prayers for your husband and your family.
Thank you for sharing, Caroline. I needed the caregiving advice.
As usual, wonderful article!!
Great article Dr Fife! Many prayers and thoughts…
Once again a great article Dr. Fife!
Thanks so much for sharing. I enjoyed the humor. I needed a laugh. This information will help me going forward.