Here’s a guest blog from a friend and colleague who practices Undersea and Hyperbaric Medicine and is also a Critical Care physician. I believe that she should remain anonymous for now. However, I was inspired by the emails and texts she has sent me and thought you would be, too. She’s sending me messages off the cuff – they are “raw” and not edited by her. However, I think that is best. She uses a lot of abbreviations and when I thought it was useful, I explained them in brackets. One day at the right time, I will tell you who she is and we can all thank her properly for her courage and commitment. Here are her COVID-19 Diaries – uncensored.
–Caroline
End of the COVID-19 Diary… For Now.
The last day in the unit was a tough day. I have the sickest patients in the icu. Five have COVID-19. Four are being proned. Their chest X-rays are complete whiteout. I’ve been ventilating one at peeps of 24 FiO2 100% for a day now. My nurses were unsettled. The previous night had been rough with four prone patients all dropping their sats and dislodging tubes, cuff leaks etc. I’m constantly juggling sedatives and narcotics, working around the dwindling supplies in pharmacy. We’re blowing through sedation medications because young patients need a lot of sedation.
Thoughts about CPR on COVID-19 Patients
The nurses told me that they were concerned about having to code these patients. As I thought it through this question, I realized that if we take the patients off the ventilator to bag them and then do chest compressions, as per usual in a code, we will aerosolize the virus all over the room, showering and contaminating every person in that room. Furthermore, we will lose the positive pressure in the lungs by taking them off the ventilator.
When you think through it, the patients are so hypoxic, that if they have a cardiac arrest, it will likely be due to respiratory failure. So I feel it is reasonable to offer a chemical code and electrocardioversion, if appropriate. It is my understanding that the ethics committee is trying to work out how to address these issues but it is so complex in nature that it’s taking time to sort through it. In the ICU we don’t have the luxury of time so until someone has better advice, I’ve made my plan.
Preparing families for the Worst
I had to prepare the family members of my patients that it’s likely their loved ones are going to die. I had to tell a child that his grandfather may not survive this disease. I had to call a woman who’s sister is intubated in the ICU that she needs to prepare for the worst. She tells me the other sister is currently in the ER with covid. I had to call a wife to tell her that her critically ill husband – a physician, is a hero. As I prepare her for the worst, I can hear her coughing from her own COVID-19 infection.
It’s been difficult physically and mentally, but being able to actively care for patients is actually a blessing. One of my friends is a great surgeon and he’s really struggling with the current situation. Surgeons are like thoroughbred racehorses horses. They have lots of energy and are they love to run – which in their case, means to operate – courageously making split decisions. In the COVID-19 crisis, they’re being held back for “emergencies only.” Imagine a racehorse, tacked up and in the starting gate, a bundle of nerves waiting for the gate to open and THEN . . just left standing there . . . COVID-19 may be harder on them than me. However, more of us are getting sick. Four hospitalists have COVID-19 now. We are all in our 30’s to 60’s with few medical problems – which ought to be encouraging, except as a group, we are just like the patients on ventilators lying prone in the unit.
I’m home now
It is so surreal. I finally got home before dark and it’s Spring!! There trees are budding and the flowers are blooming. The daffodils are so cheerful. It’s beautiful outside. Inside the ICU it is abysmal.
I slept well last night – for once, no 3 AM wake up with heart pounding and searching the literature for the latest in COVID ARDS management. Joined the morning COVID-19 conference call where the docs do a quick report on all COVID-19 patients. During those calls, we talk about the patients in terms of their physiology. Although we may know very little about them personally, we know them down to the smallest detail medically. We are seeing the limits of what the human body can handle from an acidosis, hypoxemic, life support standpoint. Even if, on rounds we discuss them as “cases,” we care about them as people and all of us become deeply attached to them. Even when we try to take a break from the ICU, we can’t stop thinking about them. The intensivist taking over for me told me to stop checking on their charts from home. I promised her I would stop obsessing, but I had to know if they survived the night. Most intubated COVID-19 patients don’t make it. The mortality for intubated patients is about 85% so by that math, I will lose at least 3 of them. Although yesterday I prepared their family members for bad news, today all four are miraculously still alive.
All of us have the same routine when we get home – which I think of as a mix between a Robert Frost poem and the movie “Silkwood.” We enter our houses through the “door less traveled,” strip down and make a beeline for the shower to decontaminate. I said hi to my family from a distance. My amazing husband has handled all household and childcare needs and kept everything under control while I’m quarantined for their protection.
What to do now? Probably some laundry, sterilize my scrubs from work. I checked in with my colleagues and so far, they’re all doing ok. I’m praying for them, we all are praying. Got some odds and ends together to make my stay in quarantine more comfortable. I won’t return to the front lines for a bit now. I may still write a daily log, because maybe it is helpful just to document a typical day. And, I take my temperature every day.
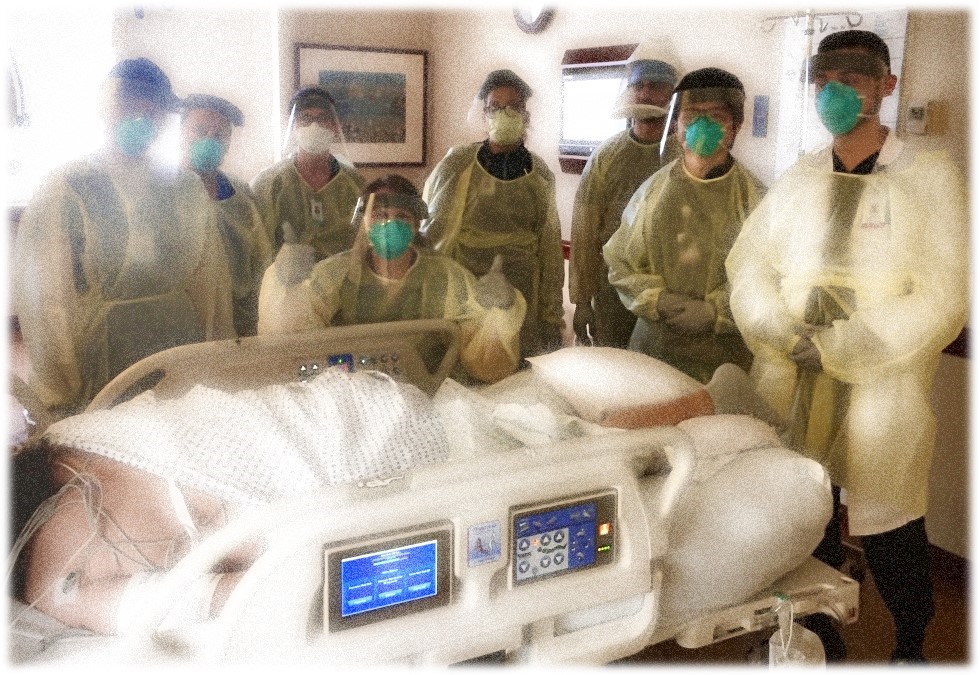
What heroes really look like.

Dr. Fife is a world renowned wound care physician dedicated to improving patient outcomes through quality driven care. Please visit my blog at CarolineFifeMD.com and my Youtube channel at https://www.youtube.com/c/carolinefifemd/videos
The opinions, comments, and content expressed or implied in my statements are solely my own and do not necessarily reflect the position or views of Intellicure or any of the boards on which I serve.



Thank you Caroline for sharing this…I shared it with my Facebook friends and family today…all 7 days. I really appreciate the writer’s sharing a real life experience and all of the candid thoughts and emotions…I really connected with this writer on every level from bedside to family experiences.
I’m glad that you shared this helpful info with us.
This surely helps many people.
Thanks a lot.
HealthForce Training Center, Inc.
https://www.healthforcetrainingcenter.com/