This article was provided by my friend and colleague, Julio R. Garcia RN, WCC, ACHRN, Program Director for the Center for Wound Care and Hyperbaric Medicine at Springhill Medical Center. “Helmet-based ventilation” may become even more vital as battles continue with the FDA regarding the use of Hyperbaric Oxygen Therapy.
Additionally, the most recent on-line issue of JAMA, an article reviews the mortality rate of patients with COVID-19 acute hypoxemic respiratory failure who received helmet based oxygen (among other strategies). The study showed that when compared with standard oxygen therapy administration methods, treatment with helmet based oxygen (in addition to some other options) was associated with lower risk of death.
–Caroline
When I first started seeing the reports out of Italy in March, I noted the “bubble helmets” on the news reports being used on the patients. This intrigued me because I recognized them as we utilize these “helmets” in multi-place operations for hyperbaric medicine. The device encloses the head and neck utilizing a clear vinyl helmet/hood and a neck ring/collar for a two-piece delivery system for Continuous Positive Airway Pressure (CPAP). You can control the gas mixture while providing the positive pressure to the lung. Positive pressure is a resistance from air pressure which helps to inflate and recruit more of the alveoli for breathing and gas exchange. The pressure, which can be provided by the helmet system, can be anywhere from 5 to 20 cm of H2O pressure. This is superior to traditional CPAP or BiPAP because you do not have the usual interface to deliver the therapy. With the masks, you can have leaks around the masks, pressure injuries to the face from tight fitting masks and escape of expiratory plumes which may spread the COVID-19 virus. The problem is teaching an old dog a new trick…no one outside of the hyperbaric medical field routinely uses these helmets, so healthcare providers are leery of their use.
A New Use for an Old Technology
This is not new technology. It is no different than providing traditional CPAP or BiPAP, it is simply a different way to deliver the therapy. There are published papers in medical journals of its effectiveness in 2010, 2016 and 2020. The University of Chicago is one of the leading researchers and utilizers of the therapy in the country. In doing research to find out more about the therapy, I came across a helmet-based ventilation website, and discovered a wealth of information on guidelines for the deployment and criteria of use of the therapy. I shared this information with our incident command and medical staff for review and consideration. Then we tried it.
One Patient’s Experience
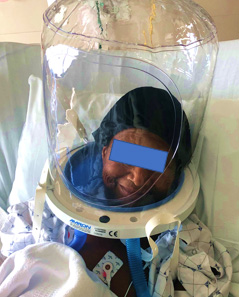 An elderly patient was admitted through the emergency department with shortness of breath and difficulty breathing. She had a low-grade fever and symptoms had been present for a week. She had a history of congestive heart failure, so this was not an unusual event for her. She was admitted to the hospital and found to be COVID-19 (+). Her status gradually became more critical. Her respiratory rate was consistently in the mid 30’s to low 40’s breaths per minute while inspiring 100% oxygen via a non-rebreather mask (NRB). Her body was having a difficult time maintaining adequate oxygen saturation levels despite being on 100% oxygen.
An elderly patient was admitted through the emergency department with shortness of breath and difficulty breathing. She had a low-grade fever and symptoms had been present for a week. She had a history of congestive heart failure, so this was not an unusual event for her. She was admitted to the hospital and found to be COVID-19 (+). Her status gradually became more critical. Her respiratory rate was consistently in the mid 30’s to low 40’s breaths per minute while inspiring 100% oxygen via a non-rebreather mask (NRB). Her body was having a difficult time maintaining adequate oxygen saturation levels despite being on 100% oxygen.
By day 3 of her admission, her oxygen saturation levels were dipping as low as 91% on 100% oxygen supplementation. She was running a marathon while resting in bed and running out of strength. She received convalescent plasma in hopes of trying to arrest the infection, but continued to deteriorate. A room air trial (taking her off oxygen therapy) revealed oxygen saturation levels of 72%. Chest x-rays showed her lungs were getting more congested.
Pulmonology decided to deploy the use of the Non-invasive Positive Pressure Ventilation (NIPPV) helmets. The results were near-immediate and dramatic. We were able to quickly wean the patient from an elevated fraction of oxygen of 100% by NRB mask to a fraction of oxygen of 0.5 or 50% with 5 cm of H2O of positive end expiratory pressure (PEEP). Her respirations became less labored, and she stated it was easier to breathe. Within 24 hours, she was out of the positive pressure helmet and was able to be placed back on a nasal cannula.
Inexpensive, Easy and Potentially Game-Changing
This response may not be typical but it sure made a difference to her. The studies show a 20% decrease in mortality and an approximate 40% decrease in the need to intubate. This is an outstanding therapy to deploy in light of the resources available and trying to keep patients from ending up on the ventilator.
I have received calls from around the country inquiring about the therapy and the limited success we have had asking how and when to utilize the therapy. Not every patient is a candidate for the NIPPV helmet, but it can have a positive effect on the outcome of a patient. It is inexpensive and easy to deploy. It allows for the patient to be able speak to and watch TV while still receiving oxygen and positive pressure therapy because it does not utilize a mask interface. It gives us another weapon in our arsenal against the COVID 19 virus.

Dr. Fife is a world renowned wound care physician dedicated to improving patient outcomes through quality driven care. Please visit my blog at CarolineFifeMD.com and my Youtube channel at https://www.youtube.com/c/carolinefifemd/videos
The opinions, comments, and content expressed or implied in my statements are solely my own and do not necessarily reflect the position or views of Intellicure or any of the boards on which I serve.



