There’s increasing interest in Vitamin D. I became focused on this after a series of patients who failed to heal operative wounds. I found their Vitamin D-OH levels were in the teens (in some cases, single digits) when 30 is the lowest value we want for wound healing. Once I got their Vitamin D levels up to 30, the wounds healed. We also know that there’s a relationship between low Vitamin D and depression, ad well as death from COVID-19 infection.
I suspect Vitamin D levels are dropping in part due to the restrictions of COVID-19, which have kept more people inside. I’ve increased my Vitamin D intake to 8,000 units a day ever since the Canadian study indicating that the currently accepted “minimum daily requirement” was incorrectly established. There seems to be an increasing interest in the topic of Vitamin D, so I’m reposting some past entries.
–Caroline

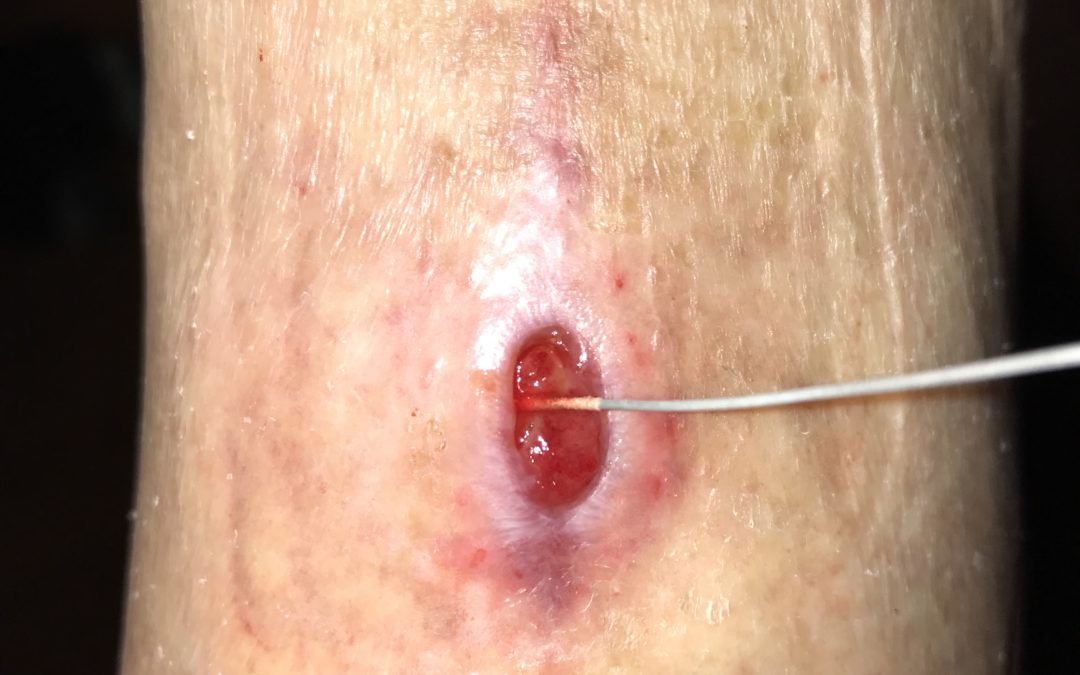
This is a 70 year old man who underwent surgery for a ganglion cyst two months before he was referred to the wound center. Ten days later when the sutures were removed, the wound just fell open. He underwent debridement and closure, and the same thing happened. These photos show a pale wound bed that has no granulation tissue. The circle I marked with a sharpie on the top of his foot is the total area of undermining which is HUGE. There is just no healing going on:

You may be thinking, “He probably has arterial insufficiency,” and we need to evaluate him for that. On the first visit of every patient, I perform an arterial screen with skin perfusion pressure (SPP) or transcutaneous oximetry. His SPP was totally normal, as was his pulse volume recording. If you still think he might have arterial disease, check out this video. Yes, that’s the Dorsalis Pedis artery pulsating in the wound bed. At first I thought it was a muscle fasciculation, but then I realized, NO! That’s his atrial fibrillation!
He’s got pale, pale tissue, and he’s making no effort to grow blood vessels. His tissue is so poor it just falls apart, and that’s why he has to much undermining. What does your “wound whisperer” instinct say about this wound? It said to me, “nutritional deficit.” So, I drew a Vitamin D level. Here’s the result:

His Vitamin D 25-OH is 17 ng/mL Anything less than 20 ng/ml is deficient. I prescribed 50,000 units once a week for 12 weeks, as well as 15 minutes of sunshine a day. Many patients are like prisoners – even in Texas, they get almost no sunshine because they are either in facilities without easy access to the out of doors, have been in and out of the hospital, or have been told to stay out of the sun.
Check out this photo of the wound after only THREE WEEKS of Vitamin D supplementation. It’s a different wound entirely!

He has almost no undermining, and the wound bed is filled with granulation. After two failed operations, in three weeks he is healing, with only one small intervention.
There’s a Vitamin-D deficiency epidemic. I could show you a case like this every single month. It may be the most common reason for surgical wound dehiscence. More than 80% of the levels I have drawn in the past year have been low – and I mean really, really low – and every single patient with a low level was already taking Vitamin D supplements. What really scares me is that I have only been paying attention to this for the past 2 years. How many others have I missed? The high-dose Vitamin D I prescribed wasn’t covered by his prescription drug plan, but it cost less than $12.00 for a 3-month supply. On the other hand, the test to check his blood level cost $350.00. I know this because the patient got a letter from Medicare telling him that the test wasn’t necessary. Drawing Vitamin D levels is not considered “evidence-based,” even for a surgical dehiscence. However, a recent issue of JAMA might loosen up the guidelines since supplementation appears to reduce the rate of cancer recurrence.
And don’t overlook the other half of the prescription – 15 minutes of sunshine a day. Many patients have their days and nights reversed, which might have something to do with the increasing frequency of severe depression among the elderly. I tell them they have to enjoy their morning coffee or juice on the porch, otherwise the treatment won’t work, and the next thing I know, their depression is dramatically better. Really good surgeons are increasingly having problems with wound dehiscence – which is actually THE most common type of wound among Medicare patients (much more common than diabetic foot ulcers or venous ulcers). One of my favorite surgeons has had three of these cases in the past 6 months. He recently told me that I was a “genius.” Now I am struggling with whether I should confess to him that my “genius” is just $12.00 worth of vitamin D and morning coffee in the sun. I will probably tell him, but first I will whisper it to you.

Dr. Fife is a world renowned wound care physician dedicated to improving patient outcomes through quality driven care. Please visit my blog at CarolineFifeMD.com and my Youtube channel at https://www.youtube.com/c/carolinefifemd/videos
The opinions, comments, and content expressed or implied in my statements are solely my own and do not necessarily reflect the position or views of Intellicure or any of the boards on which I serve.



Is the Vitamin D PO or IM or SC?
Check the patients in senior facilities or those with nursing care. Food is NOT ORGANICALLY GROWN. Most is highly processed and it is known that Vitamin D is depressed by as I recall up to 20% by glyphosate. Glyphosate is highest in Wheat, Barley, Legumes and Cane Sugar. It is used as a dessicant prior to harvest even on non-GMO labeled crops.
Stuff needs a full ban on use of human food supplies and perhaps more.
Did anyone see 2020 years number of returning California Monarch butterflies? Glyphosate is a biocide.
Dear doctor Fife,
I read your article
https://carolinefifemd.com/2019/04/15/wound-whisperer-shhhh-my-secret-treatment-for-a-surgical-wound-dehiscence/
I kindly ask You if a sarcoma old patient in good shape but with a similar dehiscent wound (8 cm length) could face a chemotherapy.
Thank You
Best regards
Emmerildo
My child had a accident 2 years back, plate with 8 screws in his arm had a skin craft now there is a open round wound, guss is coming out doesn’t close,and he lives in America Florida