Wounds are a symptom of disease, and usually the first disease we have to rule out in patients with lower extremity wounds is poor perfusion. Arterial disease is the most common reason, but not the only one. I rely on skin perfusion pressure (SPP) to determine whether the perfusion specifically to the area of the wound is adequate. I am going to post a series of articles explaining why I must have this machine or I can’t provide adequate care.
–Caroline
Because skin perfusion pressure is FAST and sometimes we need to know fast…
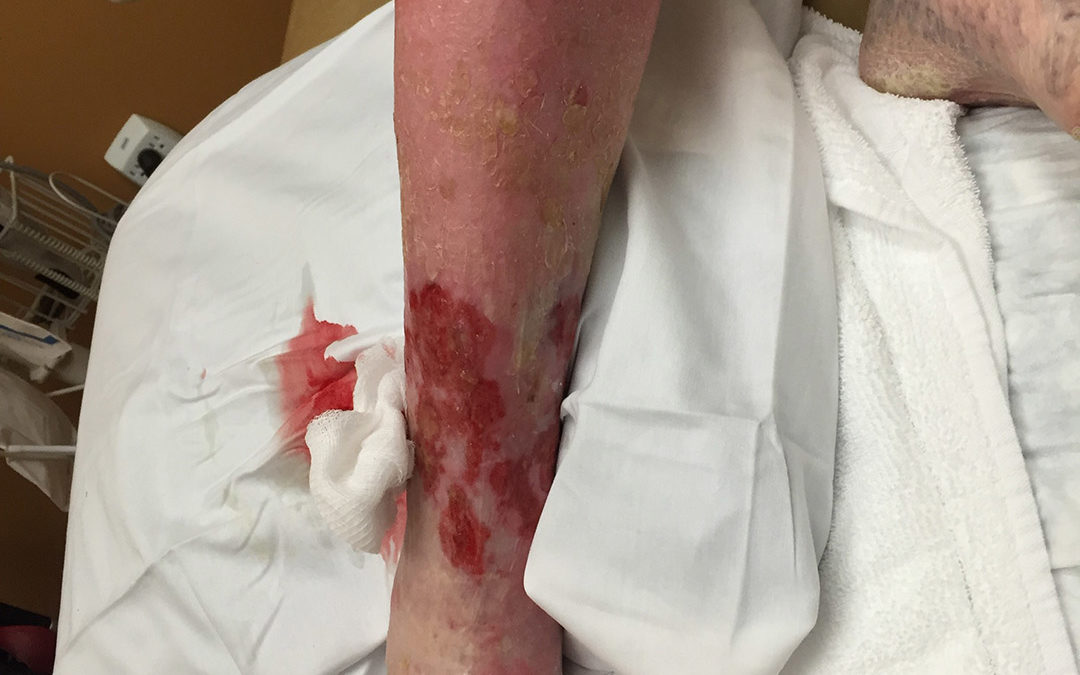
This is an alert woman in her 90’s who still lives alone. She has had a circumferential leg ulcer for 4 years and severe leg pain. She has been to a series of physicians and some months before this photo was taken, she was admitted for IV antibiotics because of her “cellulitis” (redness of her leg). The redness did not improve with intravenous antibiotics. She was also treated with compression wraps at another wound center.
Because her foot and leg were edematous, she was referred to one of the local vein centers and underwent a venous ablation procedure, after which she was placed in a compression stocking. Her neighbor brought her to the CHI St. Luke’s Wound Clinic in The Woodlands because she had terrible pain and had not gotten better with any previous treatments. We take arterial screening seriously here. Her skin perfusion pressure on the right foot was in the single digits and her pulse volume recording (SPP) was FLAT. This indicates that she has almost no flow to the right leg. And that explains why her leg is red. She has ischemic rubor (which was mistaken for cellulitis).
I was so worried about her arterial status that she was emergently admitted to the CHI St. Luke’s hospital in The Woodlands and the following day, Dr. Sanjaykumar Patel stented a severe iliac artery occlusion. She had a very proximal arterial occlusion and that’s why she had ischemic rubor over nearly her entire lower leg (not to mention having rest pain). Over a period of many weeks, she healed this circumferential ulcer with gentle compression. (I like to use Coban 2 layer LIGHT in these patients. It’s only 20 mmHg of compression but in her case that was enough.) This little lady was able to continue living independently.
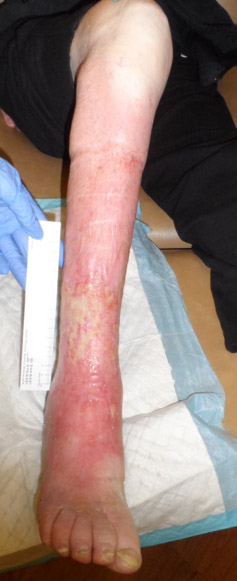
Although this sweet lady did not have diabetes, she did have a major risk factor for arterial disease – namely — advanced AGE. Nevertheless, none of the half dozen clinicians who saw her thought to do an arterial screen, including the doctor who did her venous ablation. Why is this so hard?
What do we learn from this?
- I admit it, skin perfusion pressure should not have been necessary in this case because the history and physical examination should have alerted everyone to the fact she had arterial disease.
- SPP was confirmatory so that Dr. Patel could rapidly take her to the cath lab without pausing to do any other studies.
- This poor woman suffered pain unnecessarily for months, had a venous ablation that could not help an arterial ulcer, and got hospitalized for IV antibiotics she didn’t need– all because she didn’t get a proper arterial assessment. (Let’s not even talk about the fact she was put in compression bandaging without proper arterial assessment.)
I can’t be a wound care doctor without skin perfusion pressure, and apparently neither can anyone else.
–Caroline

Dr. Fife is a world renowned wound care physician dedicated to improving patient outcomes through quality driven care. Please visit my blog at CarolineFifeMD.com and my Youtube channel at https://www.youtube.com/c/carolinefifemd/videos
The opinions, comments, and content expressed or implied in my statements are solely my own and do not necessarily reflect the position or views of Intellicure or any of the boards on which I serve.