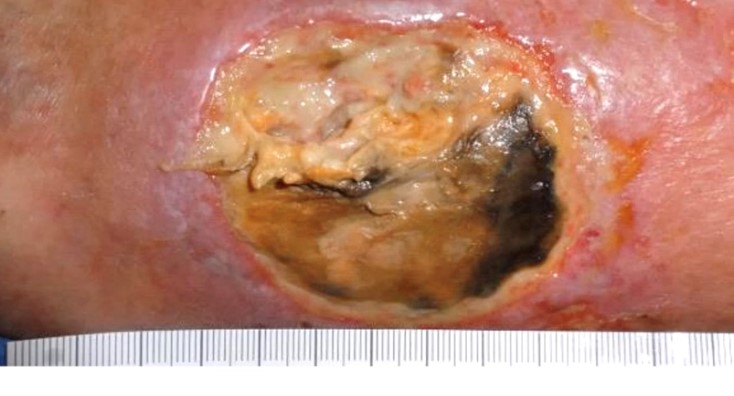
This is a man in his mid-eighties with severe peripheral edema and a nasty looking leg ulcer that’s been present for about 2 months. His edema began 2 years ago, some weeks after his wife died. It turns out that he’s lost at least 20 lbs. over the past year. When I ask him what he eats on a typical day, he’s getting very little protein. He doesn’t cook for himself, so he eats a lot of packaged food. He developed this large leg ulcer after minor trauma.
Venous ulcers are NOT this necrotic, so I assumed he had some arterial disease, pyoderma gangrenosum or perhaps a T-cell lymphoma. He didn’t have claudication or rest pain. My skin perfusion machine came in handy again – his SPP was completely normal and he had a good biphasic pulse volume recording indicating that he had good pulsatile flow to his leg so the problem wasn’t arterial. I did a biopsy and it was typical for a necrotic ulceration.
I initiated routine wound care including compression bandaging to control the edema. I also asked him to take 2 packets a day of Arginaid. I suggested that he make some changes in his diet in order to get more protein, and to take a multivitamin. His edema was in part due to his poor protein intake.
He healed with compression bandaging and improved nutrition. As best I can tell, this ulcer occurred simply because his nutrition was so bad, his tissue just fell apart after minor trauma. Be careful debriding ulcerations in patients with very bad nutrition. Give them a few days or weeks to turn their nutritional status around before you further traumatize the area, or you will just make the ulcer bigger. (We don’t talk about that enough.)
–Caroline

Dr. Fife is a world renowned wound care physician dedicated to improving patient outcomes through quality driven care. Please visit my blog at CarolineFifeMD.com and my Youtube channel at https://www.youtube.com/c/carolinefifemd/videos
The opinions, comments, and content expressed or implied in my statements are solely my own and do not necessarily reflect the position or views of Intellicure or any of the boards on which I serve.