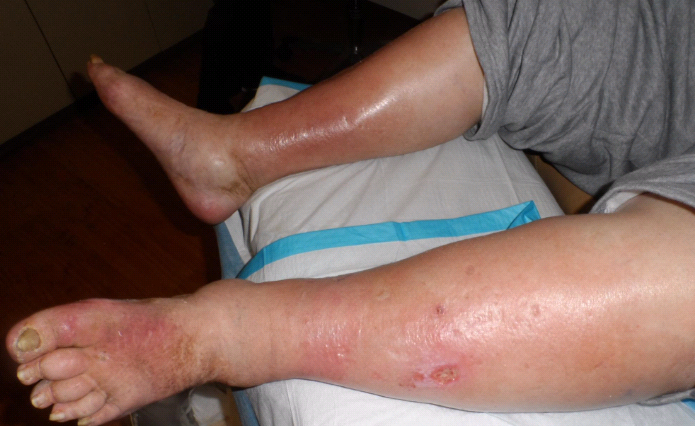
This is a 61 year old patient with weeping legs due to edema from heart failure. When I first saw her, I did arterial screening with skin perfusion pressure and her SPP values were 54 mmHg and 60 mmHg with a reasonable pulse volume recording, which means she doesn’t have peripheral arterial disease. (PAD might be the only problem she doesn’t have.) Because her arterial inflow was good, I did a trial of compression bandaging and she tolerated it. I thought maybe I could get her leg weeping under control as an outpatient by working with her cardiologist – but her Medicare Advantage plan only authorized TWO home nursing visits for compression bandage changes. She lives 45 minutes away and transportation is a big problem.
Since her Medicare Advantage plan won’t provide skilled home health services and she can’t drive to my clinic twice a week, I had to send her to the ED to get admitted. I will admit that she probably would have needed admission sooner or later for her heart failure, but when she gets discharged, what am I going to do with her? I ordered garments (Circaids) because at least those can be applied at home by her caregiver, but I don’t think she or her caregiver are going to be able to manage her leg weeping without compression bandaging.
This is not unusual. I have a patient with quadriparesis who’s getting NPWT on his sacral and ischial pressure ulcers – and Medicare Advantage won’t provide skilled home health services to change his NPWT. That means that a man paralyzed from the neck down is going to have to come to see me two or three times a week for his NPWT change because his so-called Medicare “advantage” plan won’t provide skilled home health services. I could stop NPWT and just hope for the best about his deep ulcers. Nothing about that is an “advantage.”
I once thought that Medicare Advantage was an opportunity to improve in the way that patients with chronic wounds are managed. However, rather than developing practical and evidence based policies, MA patients are suffering from the Nancy Regan “just say no” approach to services. Home health services have been abused in the Medicare Fee for Service program, but NOT providing them is not the answer. It just means that I will have to hospitalize patients instead (or not provide optimal care). I promise none of my options will save money.

Dr. Fife is a world renowned wound care physician dedicated to improving patient outcomes through quality driven care. Please visit my blog at CarolineFifeMD.com and my Youtube channel at https://www.youtube.com/c/carolinefifemd/videos
The opinions, comments, and content expressed or implied in my statements are solely my own and do not necessarily reflect the position or views of Intellicure or any of the boards on which I serve.