A 78 year old woman presented with a left medial lower leg ulcer that had been present 12 weeks. She said she awoke one the morning with swelling of her left medial leg and some mild redness. She had no confirmed history of trauma. She was not on anticoagulants and her only medical problem was mild hypertension. She had no fever or chills or weight loss and the area was non-tender. Her primary doctor put her on oral antibiotics but it didn’t appear to change anything. She has no pets, no swimming pool, no aquarium, does not eat unpasteurized dairy products and doesn’t keep roses. On her initial visit she was screened for peripheral arterial disease with skin perfusion pressure. Her was >70 mmHg (normal), so she didn’t have arterial disease. A DNA assay showed no unusual pathogens.
She had a non-tender mass that was about twice the size of the lesions themselves. When the necrotic material and debris were removed, the two skin lesions join subcutaneously and underneath them I could see the mass which was greyish in appearance. You can see some of the grey tissue in the second photo. I performed a biopsy was revealed only a chronic wound. The skin bridge broke down (the wounds had always been contiguous underneath) which made one large wound.
Because she had a lot of edema, I started compression bandaging. In fact, all I really did for her was compression. In 4 weeks she had granulated and begun to epithelialize (note that the wound divided itself in half again by sending out an epithelial bridge), and in 6 weeks she was healed.
Honestly, when I first saw her, I thought she had a tumor. Now it’s clear she had a hematoma from some trauma she didn’t remember. What is worth considering about this case is the way in which these two wounds actually formed from the INSIDE to the OUTSIDE when the expanding hematoma caused ischemia of the overlying skin. I will post some more cases in which wounds clearly formed from the inside to the outside because the skin blood supply was temporarily occluded.
When you deprive the skin of the vessels that penetrate the subcutaneous tissue, it will die. New vessels can from the vessels deeper in the subcutis, and then the skin will cover it. I think it’s pretty clear that this the mechanism by which some “pressure injuries” form, which is why this case is worth thinking about. The depth of the tissue loss is determined by the size of the vessels that are occluded and whether they also supply the underlying subcutaneous tissue and muscle.
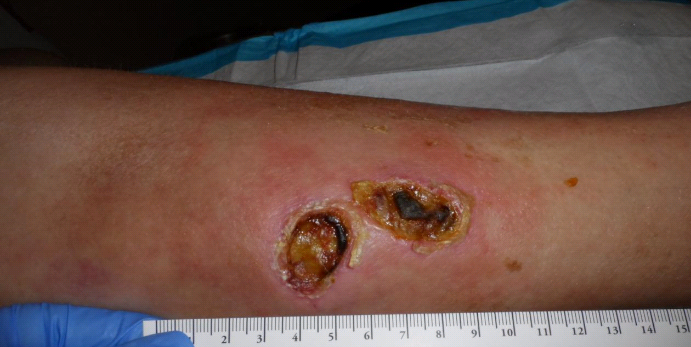
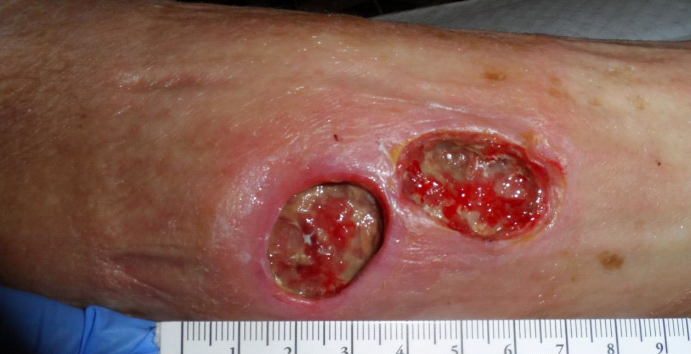 Four Days Later
Four Days Later
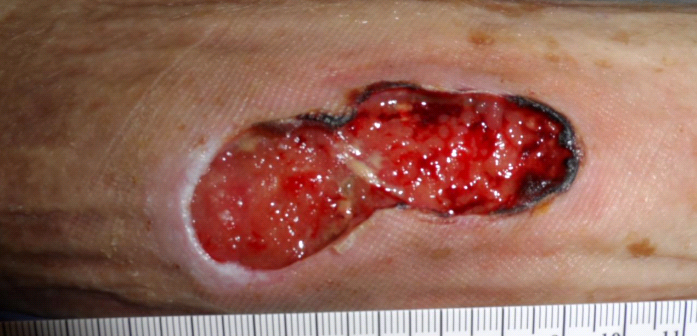 One Week After Her First Visit
One Week After Her First Visit
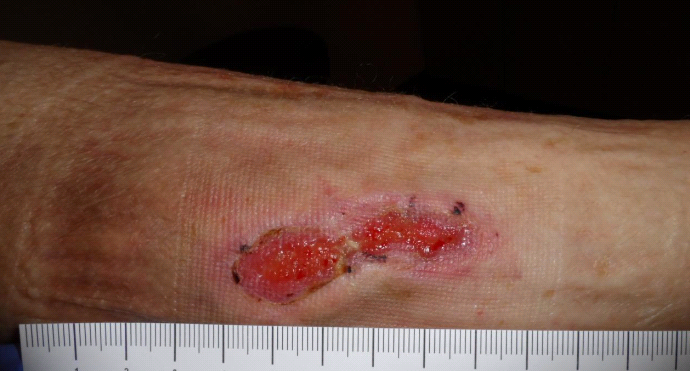 Four Weeks After Her First Visit
Four Weeks After Her First Visit
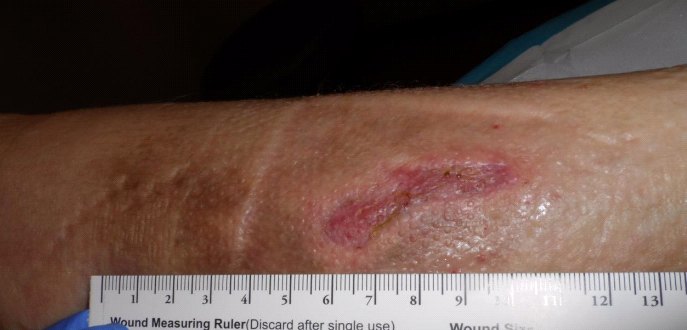 Six Weeks After Her First Visit
Six Weeks After Her First Visit

Dr. Fife is a world renowned wound care physician dedicated to improving patient outcomes through quality driven care. Please visit my blog at CarolineFifeMD.com and my Youtube channel at https://www.youtube.com/c/carolinefifemd/videos
The opinions, comments, and content expressed or implied in my statements are solely my own and do not necessarily reflect the position or views of Intellicure or any of the boards on which I serve.



Congratulations! Excellent work!
One would think that there had to have been some serious trauma in the first place but I wonder if she was just more susceptible to its effects.
I have been dealing with 4 wounds like this only mine start out as a large mass then it hardens and breaks thru the skin. Two have healed 100%, left a puckered scar tho. I just developed a new one in the past week after the lump was soft to hard under the skin for approx 4 weeks. I have been to an oncologist, surgeon, wound dr (she said only way to get rid of them is to remove the wound and the underlying “tumor” beneath it), plastic surgeon (who sys he will take all of it out with a skin removal surgery) and a general dr. I am meeting with the plastic surgeon to schedule surgery for skin removal this month and he is the only one who said he will get to the bottom of this.
Also to complicate the situation, since the lumps started, I have lost 210 pounds, I’m not trying to lose weight, I eat what I want, no medication changes, no medication to lose weight or anything. It just happened and no disease I or the physcians can come up with explains what is happening. Please respond with your opinion, I would like to know what is causing this.