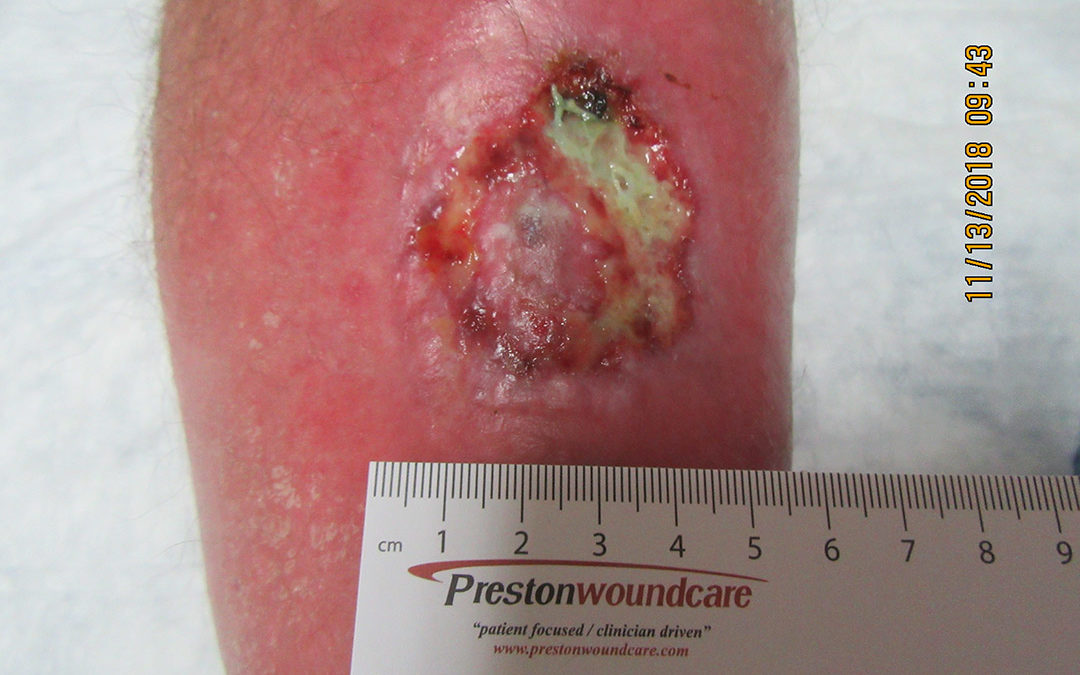
For years I have been talking about the complications of shin radiation in elderly patients. The patients all underwent radiation for skin cancer having been told that since they were old and had “circulation issues”, radiation was a better option than undergoing a large surgical excision. So far, none of the patients I have seen with radiation tissue damage have had underlying arterial disease (at least, not before they had radiation) and none even had very significant venous disease. In other words, there’s no reason to think they wouldn’t have healed a surgical excision or even a flap, but they had radiation instead – with awful results.
I don’t know if I speak for all wound care practitioners, but give me a huge surgical wound any day over a case of soft tissue radionecrosis — in terms of how long it will take to heal and whether they heal at all! Many of these patients with shin radiation have required plastic surgical flaps to handle the radiation damage, operations that were far more difficult and extensive than the original cancer surgery would have been. That’s why I’ve started the “Stop the madness of shin radiation” campaign. If you have a case like this, feel free to send it to me and I will post it (no patient identifying information please).
This case is from a colleague who prefers to remain anonymous:
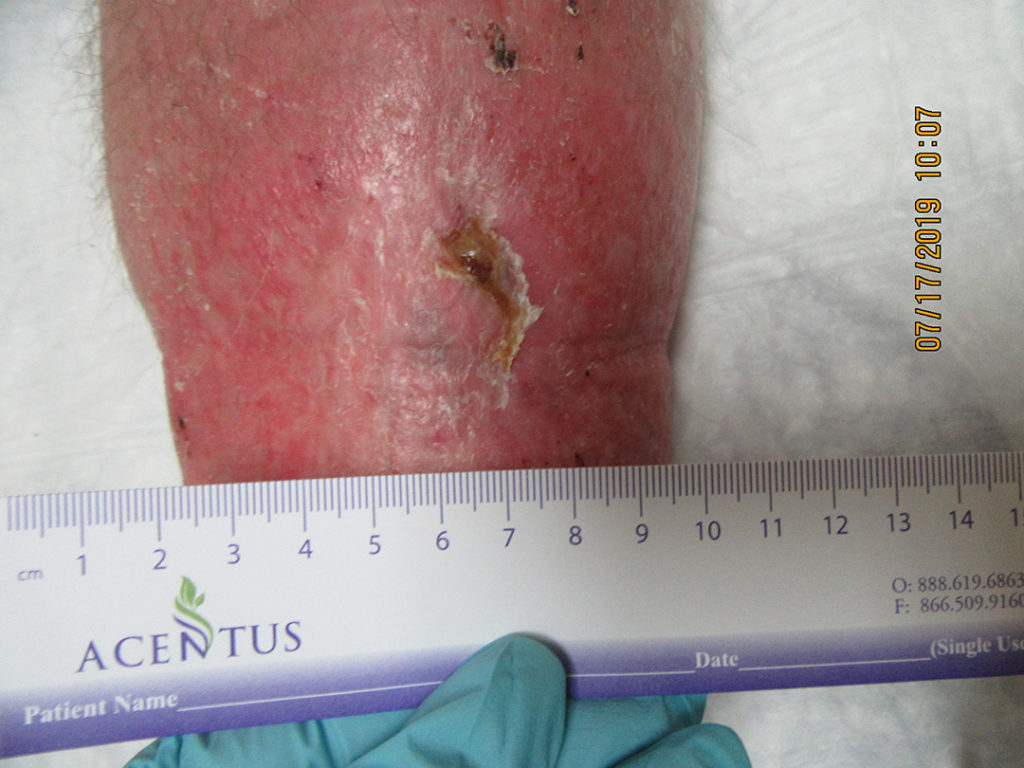
67 year old male with a history of type 2 Diabetes, HTN, obesity, and hyperlipidemia who presented with a radiation wound on the left shin after resection and radiation of a squamous cell carcinoma (SCCA) lesion (cT2N0 stage II). After resection of the lesion, he received 50Gy radiation delivered in 2.5 Gy fractions. Prior to seeing me he developed multiple bouts of cellulitis and was left with a deep leg ulcer for four months. He was eventually referred to my wound center and underwent debridement and treatment with Santyl/Mupirocin and then a few weeks later collagen dressings. He also was started on compression therapy with stockings. The wound failed to progress so he was then prescribed 30 treatments HBOT at 2.5 ATA with two 5 minute air breaks and the wound eventually came near to healing but he was lost to follow up. His arterial dopplers were within normal limits.

Dr. Fife is a world renowned wound care physician dedicated to improving patient outcomes through quality driven care. Please visit my blog at CarolineFifeMD.com and my Youtube channel at https://www.youtube.com/c/carolinefifemd/videos
The opinions, comments, and content expressed or implied in my statements are solely my own and do not necessarily reflect the position or views of Intellicure or any of the boards on which I serve.