A few months ago, a woman brought her father in to see me for his leg edema. She had intervened when his health and his mental function deteriorated dramatically. When I walked in the door, I could tell he had sleep apnea. He was falling asleep as I talked to him, his leg edema extended to the thighs, and he seemed “out of it” mentally. The daughter said the mental status changes were relatively new. A large registry study in Denmark has shown that sleep disorders are associated with a 17% increased risk for dementia. I have long been interested in the connection between the lymphatics and the cerebrospinal fluid. It is likely that SA impacts the washout of cerebrospinal fluid and that this facilitates the deposition of tau protein in the brain. (Stay tuned for more information on the relationship between the lymphatics and the brain, thanks to work being done by my friend Eva Sevick.)
I’ve talked before about the link between leg edema and sleep apnea. SA is a major factor in the pathogenesis of leg edema. I’ve decided that one of the most important questions we can ask a patient is, “Do you sleep in a chair?” The majority of my patients with profound leg edema admit that they do, and they seem equally divided between the ones never tested for sleep apnea and the ones who got tested, were found to have sleep apnea and refused to use a CPAP machine. Most of those patients have a stiff right heart and pulmonary hypertension, but that never gets worked up. When I call cardiology, they tell me the patient’s ejection fraction is normal – which of course it would be, given that the problem is on the right side of the heart and not the left.
Here’s a fantastic article about the fluid redistribution of sleep apnea as well as heart failure. The article states that even though aging and obesity are clearly the most relevant associated risk factors for sleep apnea (SA), the prevalence of SA is much higher among patients with edematous states such as end-stage renal disease (ESRD) and CHF. In patients with sleep apnea, for a variety of reasons explained in the paper, interstitial fluid increases and effective arterial blood volume (EABV) decreases – even though the patient may have an increased total blood volume. This mechanism of edema formation resulting from chronic reduction of the EABV is known as “underfilling.” This decreases renal perfusion. When renal perfusion is not maintained, the kidneys (assumed to be normal) respond as expected by reabsorbing as much sodium and water as possible. This fluid escapes the intravascular space because of a disequilibrium of Starling forces, promoting further sodium retention. In this manner, the retained fluid tends to accumulate at the interstitial compartment, instead of recomposing the EABV. Underfilling is central to the pathogenesis of edema in CHF, hepatic cirrhosis and some cases of nephrotic syndrome. I think the above is the definition of a vicious cycle. Nearly a quarter of my patients have congestive heart failure (CHF) which is a truly huge percentage. Sleep apnea is at the core of it.
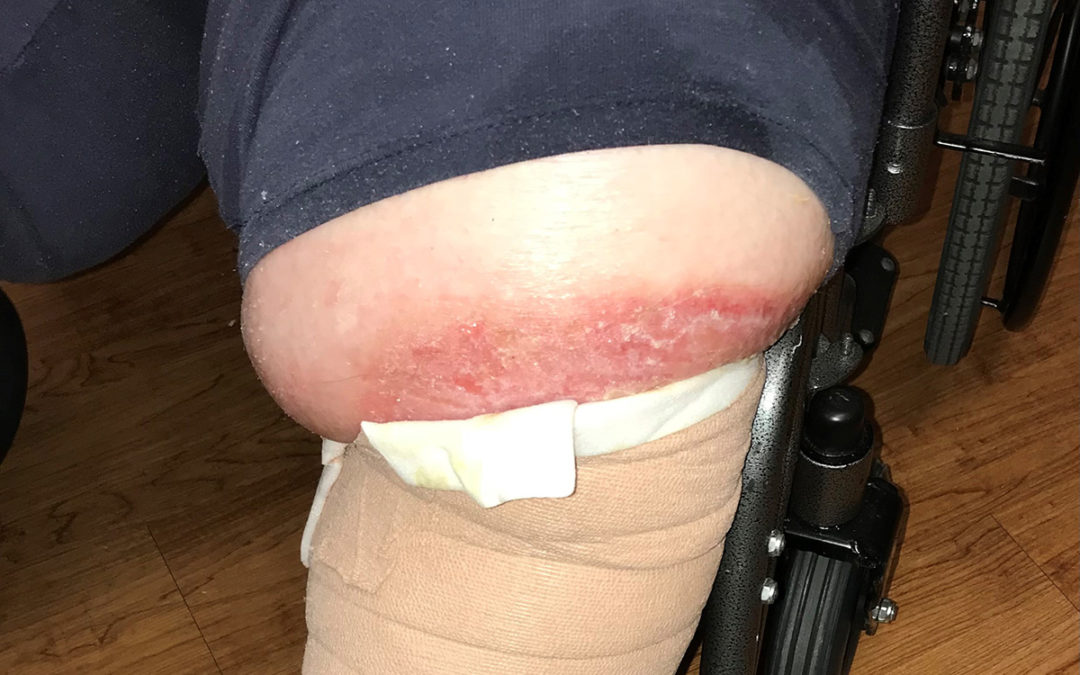
Now we have an even more compelling reason to talk to patients about sleep apnea and that is the link to dementia In any case, it’s a fool’s errand to think that we can overcome the impact of these central hemodynamic factors with compression bandages. Our patients are often edematous all the way to the abdomen. Compression below the knee just pushes all the fluid to the thighs. If you feel like you are on a fool’s errand when it comes to managing leg edema, the reason is that we are only treating the final manifestation of life-threatening systemic problems. (I want to be clear that my staff did not apply the bandage in this photo – but it explains why we are fighting a loosing battle when edema extends to the thigh.)

Dr. Fife is a world renowned wound care physician dedicated to improving patient outcomes through quality driven care. Please visit my blog at CarolineFifeMD.com and my Youtube channel at https://www.youtube.com/c/carolinefifemd/videos
The opinions, comments, and content expressed or implied in my statements are solely my own and do not necessarily reflect the position or views of Intellicure or any of the boards on which I serve.



Wow, I have sleep apnea, but it got better so I do t wear my c pap. I also have MS. My legs are swelling, esp around the ankles and calves. My family MD told me my ankles were just fat :(. I’m going back to the sleep dr this Friday. Any suggestions? I also have a pain pump and stimulator for my bladder.