This exciting series is limited to our registered subscribers only. We will NOT sell your information – and this content is totally FREE – no strings attached. We will email you if there are any exciting new publications in the field of lymphology.
The (Mostly) Complete Guide to Lymphatic Anatomy Part 1: Why We Need Lymphatic Imaging and a Synopsis of What We Have Learned From it So Far
by Caroline Fife, M.D. | Nov 10, 2022 | Guide to the Lymphatic System | 1 comment
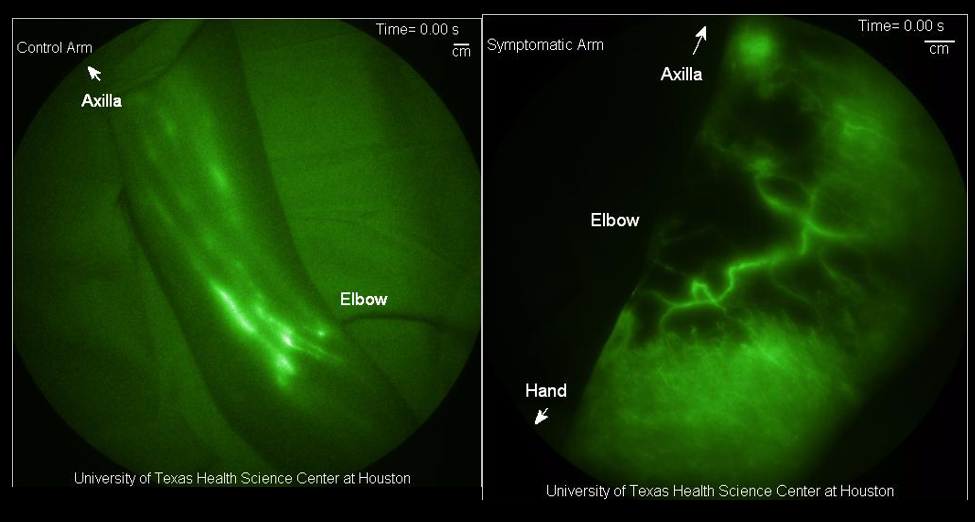



As a lymphedema therapist, I’m thrilled that there’s NIRF-LI to help diagnose and guide treatment for lymphedema patients. It’s truly a game changer. Yet, here in Tucson, Arizona my colleagues and I have been looking, unsuccessfully, for over a year for a physician who would make this available to our patients, and theirs.
Any ideas, guidance, suggestions, contacts?
I so appreciate this generous sharing of your work.