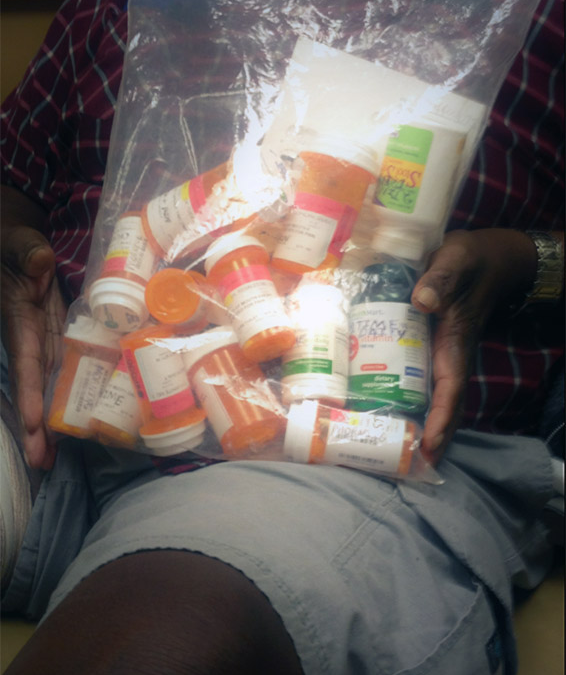
I haven’t been able to get this patient off my mind. He’s a kind and likable man who was active in his church and living independently, despite an above-knee amputation on one side and chronic lymphedema of the other leg. He had made a living as a truck driver until he developed the ischemia that took one leg. He only had about a third grade reading level, and once brought the large sack of his medications to the office to ask me what they were for. I went through all of the medications and wrote in simple terms on each bottle what they were for and how to take them. His frequent visits to the wound center for compression bandaging kept him out of the hospital and minimized the tendency for the leg with lymphedema to break down into draining wounds. His visits, compression garments and his many medications were covered by his Medicare Fee for Service (FFS) plan and his Medicaid. It was going well, until he got a phone call from someone advertising a Medicare Advantage (MA) plan. The person on the phone told him all about the “advantages” he would have with an MA plan. Unfortunately, he could not read the paperwork that they provided — which he signed.
Do I need to tell you the rest? He suddenly had out-of-pocket expenses he could not afford, his visits to the wound center were no longer covered, and I stopped being able to see him. My sweet front desk employee tried valiantly to get him back on a Medicare FFS plan, making phone calls between her other responsibilities, trying to explain that he was illiterate and had been unable to read the paperwork he had signed under false pretenses. It didn’t help. The patient cried on his last visit, and so did I.
Nearly every large insurance company in the program, including UnitedHealth Group, Elevance Health, Kaiser Permanente and Cigna, has been sued by the Justice Department for fraudulently overcharging the government. Although they get paid a lot by the government for providing care to Medicare eligible patients, a recent report by the inspector general of the U.S. Department of Health and Human Services found that several MA plans, “might be inappropriately denying care to patients.” That’s old news to doctors and the patients who have been denied needed services for wound care. MA patients are paying HUGE deductibles and out of pocket expenses, and most plans will not cover treatment at a hospital based outpatient department. I’ve previously posted blogs from another patient about her experiences with what I have referred to as “Tales of the Medicare Disadvantaged.” I have warned all my patients with a traditional Medicare FFS not to be talked into an MA plan, but that’s all I could do to fight the misinformation.
Finally, Federal health officials are proposing an extensive set of tougher rules governing private Medicare Advantage health plans, in response to wide-scale complaints. A new proposed rule by the Centers for Medicare and Medicaid (CMS) focuses on protecting people from confusing and potentially misleading marketing. CMS proposes to codify guidance protecting people from misleading marketing and ensure they are not pressured into enrolling into plans that may not best meet their needs. I don’t know if it will go far enough, but at least it’s a start. You can read more in this CMS release, and this NY Times article. Unfortunately, it comes too late to help my patient.

Dr. Fife is a world renowned wound care physician dedicated to improving patient outcomes through quality driven care. Please visit my blog at CarolineFifeMD.com and my Youtube channel at https://www.youtube.com/c/carolinefifemd/videos
The opinions, comments, and content expressed or implied in my statements are solely my own and do not necessarily reflect the position or views of Intellicure or any of the boards on which I serve.



Thank you Caroline for your post regarding this issue of Medicare Advantage plans and how patients are denied coverage that would have been covered had they stayed in traditional Medicare plan. I deal with this daily with our MicroGenDX testing service which is covered by Medicare but often denied by the Advantage plans. We need more people like you to raise this problem and stop the harm it does to patients!