If you are “eligible” for MIPS (Medicare’s term for “required” to report) and you ignore participation entirely, you can lose up to 9% of your Medicare billing for the year. For most practitioners, that sufficient reason to at least check your reporting status.
It is incredibly easy to find out if you are required to participate in MIPS. All you need is to type in your National Provider Identification (NPI) number here: Check Eligibility. However, it is NOT easy to understand the report when you get it.
Eligibility requirements for the CMS MIPS program
Remember, MIPS eligibility is NOT based on where you see patients! A common misconception is that practitioners who care for patients in the home (e.g., “mobile” practitioners) are not subject to the QPP. That is a myth.
There is a lot of fine print in the MIPS eligibility requirements, and there are exclusion criteria, but to be MIPS “eligible” (“required to report”), practitioners must exceed the “low-volume threshold” (LVT) for Medicare Part B professional services. The LVT is determined from the Medicare claims billed for a TIN (tax ID number) or TIN/NPI combination.
You exceed the Low Volume Threshold (and are thus required to report) if you:
- Bill more than $90,000 in Medicare Part B covered professional services AND
- See more than 200 Medicare Part B patients AND
- Provide more than 200 covered professional services to Medicare Part B patients.
CMS evaluates clinicians (TIN/NPI combinations) and practices (TINs) for the LVT twice for each performance year. Each review analyzes a 12-month segment, and your final eligibility determination is released in December of the performance year.
Let’s assume you have entered your NPI on the QPP Participation Status website Check Eligibility. As you scroll down the page, you will see your name and practice address, and under “MIPS Participation,” your “MIPS eligibility.” Now what?
The Categories of Eligibility
Eligible as an Individual:
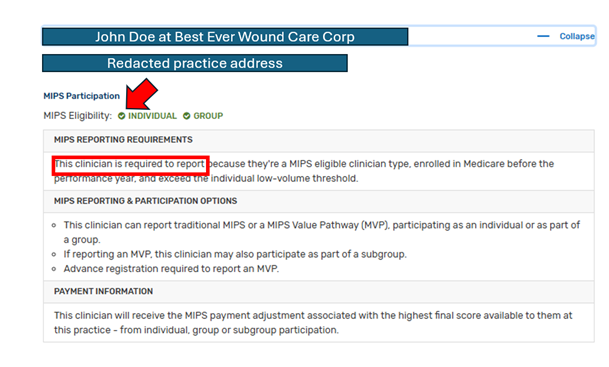
The most important thing to pay attention to is whether there is a green check beside “INDIVIDUAL,” and the sentence, “This clinician is required to report”. It will look like this:
If you are employed by an organization, you may not have to handle any data submission yourself. Even if the actual reporting is being handled by your employer, your salary or bonus might be linked to your QPP performance, so you should discuss that with your employer. You might also be participating in a MIPS APM (Alternative Practice Model). The APM may be reporting data on your behalf.
The important point is that if you are eligible for MIPS, it’s up to you to understand what, if anything, you need to do so that you do not lose money. If you do not understand what you need to do, I recommend that you contact a MIPS consultant (I strongly recommend Linden Healthcare Consulting).
Individual MIPS eligibility is tied to a TIN/NPI combination, so if you practice under multiple TINs, you should review your eligibility at each TIN listed.
Eligible as a Group
Next to the important Individual eligibility indicator is a Group eligibility indicator that looks just as important – IT’S NOT. This is the most confusing part of eligibility: Individual eligibility = required to report; Group eligibility = an optional convenience.
Group eligibility is based on the same Low Volume Threshold as individual eligibility ($90,000/200/200), so most groups that bill Medicare will show as eligible when you add up every NPI under the TIN. However, there is NO REQUIRED GROUP REPORTING in MIPS. It’s simply an option for practices who want to submit one report to cover everyone in the group instead of having to submit multiple individual submissions.
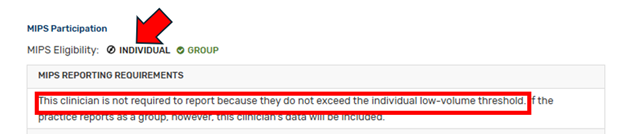
Here’s an example of a practitioner who is not required to report MIPS, but who practices at a Tax ID that could choose to report MIPS (note there is no green check by INDIVIDUAL, but there is a check at GROUP):
If you are NOT eligible as an individual but there is a green check beside “Group” – you are not required to report. This does not mean that you MUST report with a group. Yes, this is confusing, but the important point is that you are not required to report as an individual.
We could actually stop right now and call it a day, once you have determined that you are not required to report. However, nothing is that straightforward with CMS. Clinicians who are not required to report can still decide to report anyway. The clinicians who are not required to report will either be “Opt-in” eligible, or they can volunteer. Keep reading.
Opt-in Eligible as an Individual
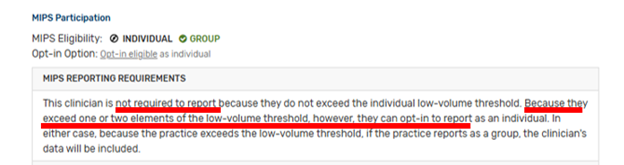
A physician is not required to report unless they exceed all 3 of the low-volume threshold criteria. However, if a physician exceeds one or two elements of the low-volume threshold, they can “Opt-in” to MIPS reporting. This is an example of the wording on the CMS website if you are an “opt-in” eligible practitioner:
If this practitioner decides to “opt-in,” then they will be treated exactly the same as the clinicians for whom reporting is mandatory. In other words, if you opt-in, and your MIPS scores are bad, you will experience a monetary penalty (meaning, you will lose some of your Medicare payments). However, if you opt-in and have a high score, you could receive a Medicare bonus.
The only reason to opt-in is to earn an incentive payment, so do not opt in unless you are certain you can avoid the payment cut.
If you are opt-in eligible, ask yourself: what would my return on investment be for opting in, and how much work will I need to do to report?
The maximum upward payment adjustment in MIPS is generally around 1-2%, so if you are not eligible (required) because you do not exceed $90,000 in charges, your maximum return will be less than $2,000, and it’s unlikely you would benefit by opting-in. The only exception to this is if you believe your charges will be significantly higher in 2 years’ time when the payment adjustment is applied – in that case, successful reporting now can be an investment in your future Medicare payments.
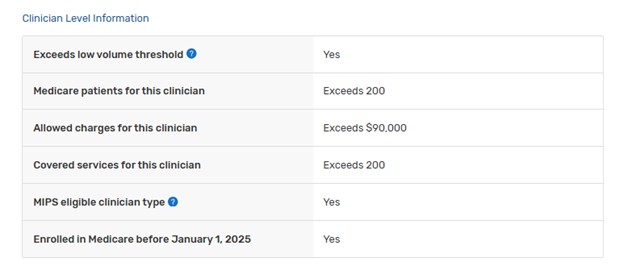
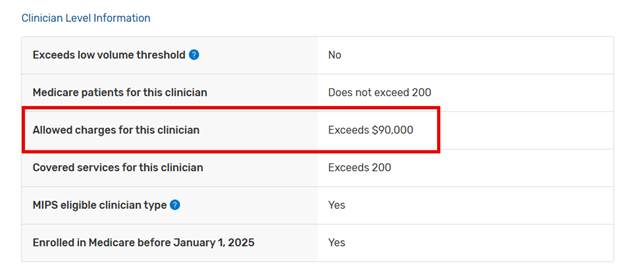
Another reason to consider opting-in is if you are not eligible (required) because you did not see 200 unique patients, but you had over $90,000 in allowed charges, like this example:
The public eligibility only shows “Exceeds $90,000,” but if that volume is high enough, even a small upward bonus can be enough to pay for the time and effort necessary to get the submission right.
The second consideration, how much work you will need to do to avoid the cut, depends on too many factors to address here. Some providers can earn a bonus very easily with very little work, but for others, opting in will almost always be a bad idea. If you’re unsure, do not opt in, or discuss it with a MIPS consultant first.
Voluntary reporting
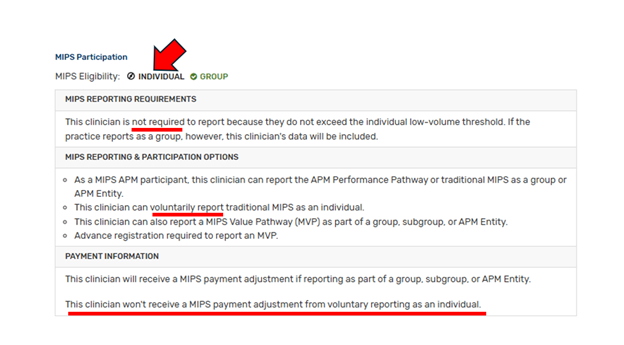
Any practitioner who is not required to report may “volunteer” to participate. This includes opt-in eligible clinicians who do not opt in, and ineligible clinicians, regardless of reason (APM QP, LVT, new to Medicare, etc.). If you choose to voluntarily report, your MIPS data will not be used to determine a payment adjustment. A good score will not earn you a bonus, and a bad score will not result in a penalty. Here’s an example from the CMS website of someone whose only choice is voluntary participation:
Why would anyone go to the time and trouble to submit data if it does not count either for or against them? Some clinicians volunteer to participate in MIPS as a “practice round,” particularly if their practice is growing fast and likely to be required to participate next year. Voluntary reporting is also a way to determine how your electronic health record (EHR) is collecting quality measure data and how any registry you are working with is performing. In most cases, though, there are more efficient ways to practice or test your systems than a voluntary MIPS submission. It is hard to make a case for volunteering.
Other Important Information to Check on the Eligibility Page
Once you have determined your reporting status, there are some other important things to check!
1, Are your practice affiliations correct?
This is far more important than you might think. The Department of Justice (DOJ) released information about an individual indicted for health care fraud who was using the National Provider Identifiers (NPIs) of four physicians without their knowledge to submit fraudulent claims for hyperbaric chamber supervision.
If you do not recognize a practice name linked to your NPI, contact the Provider Enrollment department of your local Medicare Administrative Contractor (MAC), or the MAC for the state where the incorrect enrollment is displaying.
Do not be concerned if the address listed for a practice is outdated or a secondary location. The address displayed is usually the most recent one updated in NPPES, not the primary address, and this has no bearing on MIPS participation or payment adjustments.
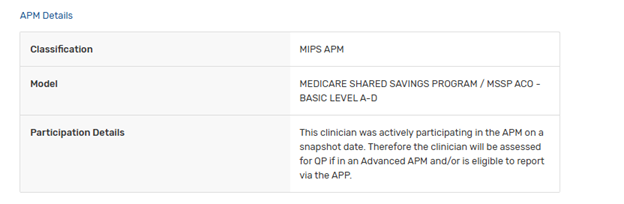
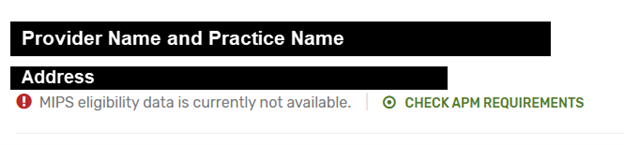
Also do not be concerned if a practice you no longer work at is still showing up. Because eligibility uses two years of Medicare data for each MIPS year, old practices can take an extra year to disappear. Additionally, if the old practice was in an ACO (Accountable Care Organization) and the ACO does not keep their participation list updated, the old practice can continue to display for years. In that case, it usually looks like this (no billing data, but an APM still listed):
Special Statuses
CMS has a LOT of different categories and special status designations (Special Statuses – QPP), each of which has implications on the way that MIPS is scored. This topic is incredibly complicated and is yet another reason to retain a consultant. I will list a few here just so that you know what else to look for on the eligibility status report.
2. Are you hospital-based?
If you are working in a hospital-based outpatient department, your status should say “Hospital-based – Yes”. This means that you furnish 75% or more of covered professional services in a hospital setting as identified by Place of Service (POS) Codes 19, 21, 22, and 23.
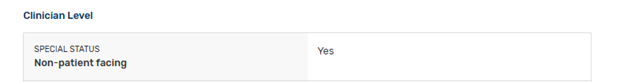
3. What does “non patient facing” mean?
If you have 100 or fewer Medicare Part B patient-facing encounters (including telehealth services), you are considered “non-patient facing.” Keep in mind that many providers who do not exceed the low volume threshold will have fewer than 100 encounters TOTAL, causing this status to display. Additionally, if you bill patient-facing and non-patient-facing codes on the same claim, CMS will consider that overall “encounter” non-patient facing.
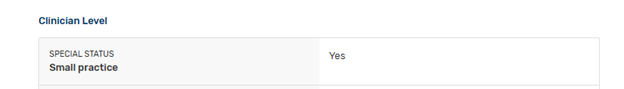
4. Are you in a small practice?
A small practice is a practice with 15 or fewer clinicians billing under the practice’s TIN during both eligibility determination periods. Being in a small practice means that you only have to do one improvement activity, you are exempt from the PI category, and quality scoring is much easier. Be aware that if your practice hires a 16th clinician (which moves you from a “small practice” to a “large practice”) the MIPS implications can be significant. You can also lose the small practice status due to turnover, even if you never had 16 clinicians billing under the TIN at any one time.
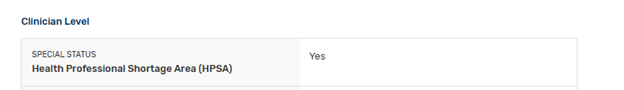
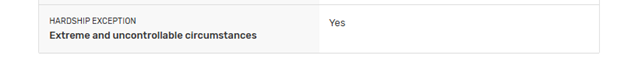
5. Do you have a special status such as practicing in a Health Professional Shortage Area (HPSA)?/6.Do you have any MIPS hardship exemptions such as “extreme and uncontrollable circumstances”?
If you were affected by certain natural disasters (fires, hurricanes, etc.) CMS will exempt you from certain reporting requirements.
6. Do you have any MIPS hardship exemptions such as “extreme and uncontrollable circumstances”?
If you were affected by certain natural disasters (fires, hurricanes, etc.) CMS will exempt you from certain reporting requirements.
The topic of the Quality Payment Program (QPP) is like a dose of Ambien, but if you don’t pay attention, you can lose some of your hard-earned money. In past articles, I have reviewed the QPP through the lens of wound care, explained the basics of how scoring works under the Merit Based Incentive Payment System (MIPS), and pointed out the sad fact that MIPS probably hasn’t done anything to improve the quality of medical care.
I totally understand the sentiment of the physician who told me that he refused to participate in MIPS because he “didn’t think it was even legal.” Believe me, I understand the frustration. However, unless you enjoy losing money, you will have to figure this out. You can see why a MIPS consultant may be needed just to explain your status, much less advise you on various options for reporting. Hopefully, at the very least, you now are able to determine whether you are required to report MIPS data.

Dr. Fife is a world renowned wound care physician dedicated to improving patient outcomes through quality driven care. Please visit my blog at CarolineFifeMD.com and my Youtube channel at https://www.youtube.com/c/carolinefifemd/videos
The opinions, comments, and content expressed or implied in my statements are solely my own and do not necessarily reflect the position or views of Intellicure or any of the boards on which I serve.