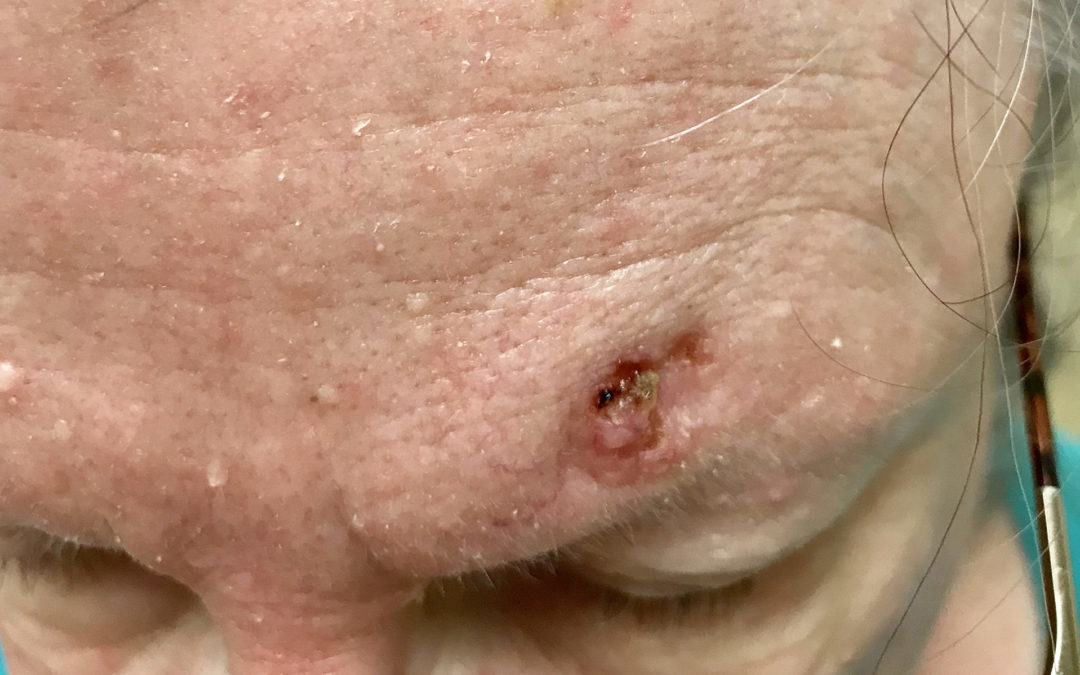
This woman had a stroke at home and was on the floor for 3 days before anyone found her, so I am treating the sacral and heel pressure ulcers which developed during that time. However, on her first visit I noticed was this pretty BIG skin cancer on her forehead. She has a Medicare “Advantage” HMO. After many weeks of leaving messages and sending letters to her primary care doctor regarding her need for a dermatology referral, I biopsied it myself and sure enough, it’s a basal cell cancer.
It’s now been 4 months that she’s been waiting to see a dermatologist. She tells me that her PCP can’t find a dermatologist who takes her Medicare HMO insurance. I’m grateful that her Medicare HMO is allowing her fairly serious pressure ulcers to be treated at a wound center, so I shouldn’t be too critical of them. However, it’s a challenge to treat Medicare “DIS-advantage” patients, because they require me to have a “peer to peer” phone call for every advanced therapeutic (and I am already very frugal in my use of them) – and sometimes they don’t approve a cellular product or other treatments that I recommend.
This is the second time that I have seen a patient whose insurance plan simply did not include a specialist they needed. I blogged about this in 2015 when a patient with a rapidly spreading neck tumor needed to see an ENT surgeon emergently and there were none on his “insurance” plan.
https://carolinefifemd.com/2015/10/20/straight-talk-tuesday-38/
We don’t seem to be discussing this in the healthcare debate. I keep hearing numbers thrown around about how many patients might become uninsured with one change or another, but no one talks about how many patients currently THINK they have insurance, but they actually DON’T. I mean, if you have a Medicare “Advantage” plan, and you can’t get a skin cancer taken off your face, it doesn’t seem to me that you have Medicare. But that’s just me.

Dr. Fife is a world renowned wound care physician dedicated to improving patient outcomes through quality driven care. Please visit my blog at CarolineFifeMD.com and my Youtube channel at https://www.youtube.com/c/carolinefifemd/videos
The opinions, comments, and content expressed or implied in my statements are solely my own and do not necessarily reflect the position or views of Intellicure or any of the boards on which I serve.



HMO’s are just pure dangerous. They dont make money when you see their doctors, only when you dont. Second, independent opinions are not possible.