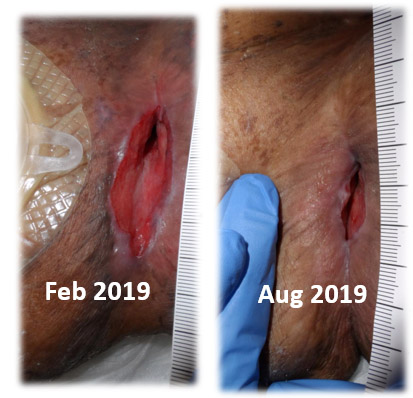
The photo above shows the un-encouraging 6-month course of a dehisced abdominal wound. There’s not much to show for all my hard work. Treatment with Negative Pressure Wound Therapy (NPWT) had absolutely no impact (and broke down the periwound skin), so we stopped. I know what’s wrong with her NOW, but I didn’t know the diagnosis 9 months ago.
The history she related was that over the past 16 years she’s had four spontaneous ruptures of her colon (one while pregnant), three re-do operations for the inevitable ostomy, and multiple abdominal hernia operations, the most recent of which resulted in a dehiscence of the midline incision. It’s the abdominal wound that has been laughing at me for so many months. She’s been told she has rheumatoid arthritis, and the prednisone she had to take caused her to develop diabetes. When I took this sad history I thought, “She must be the unluckiest person (still) alive.”
Her problems were not bad luck. It’s another case of Ehler Danlos Syndrome (EDS), which has been missed all these years. I only figured it out because a different patient took the time to return to tell me that she had been diagnosed with EDS after I missed it. Suddenly the spontaneous bowel ruptures, abdominal hernias and wound dehiscence(s) made sense. That was less than a year ago, and I have found two more EDS patients whose sad life stories are nearly identical.
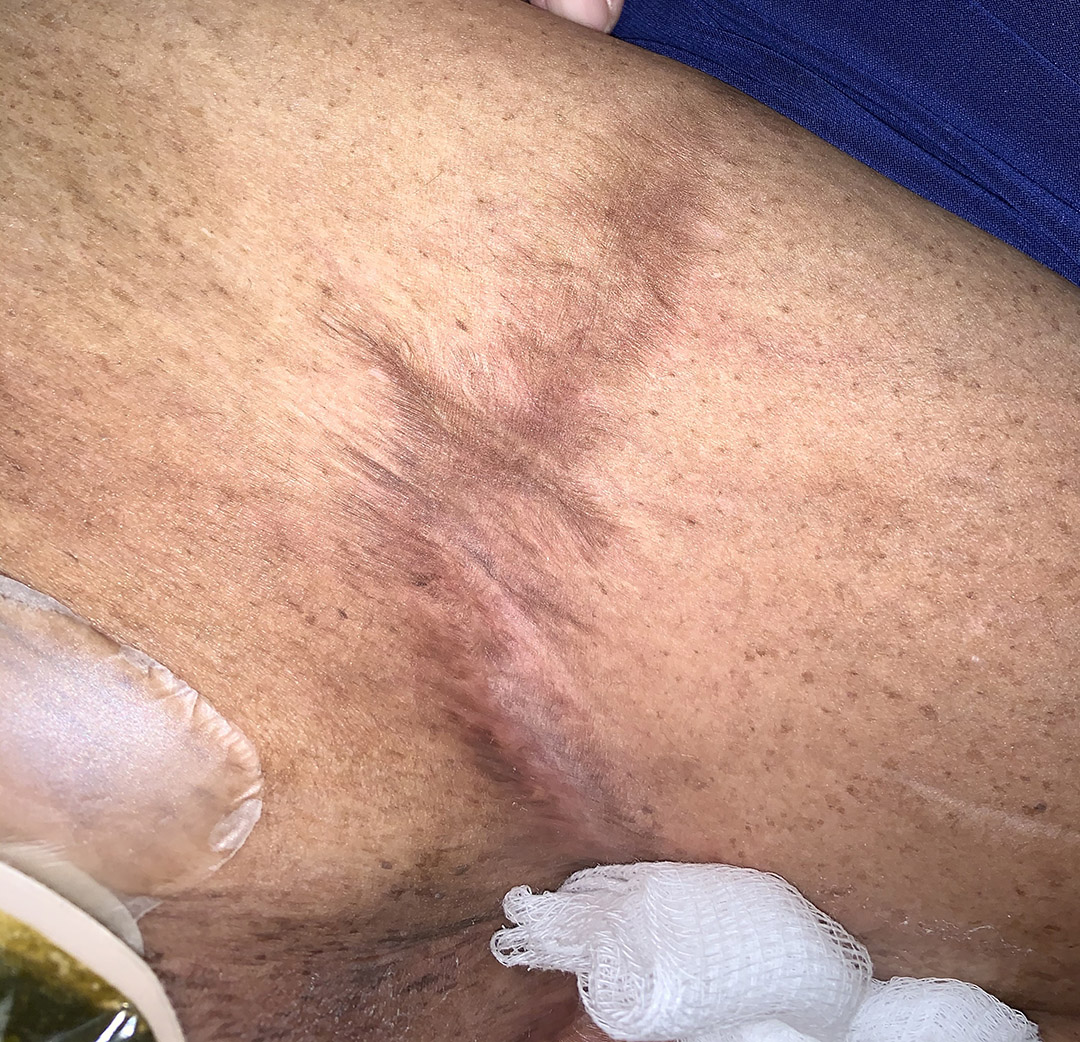
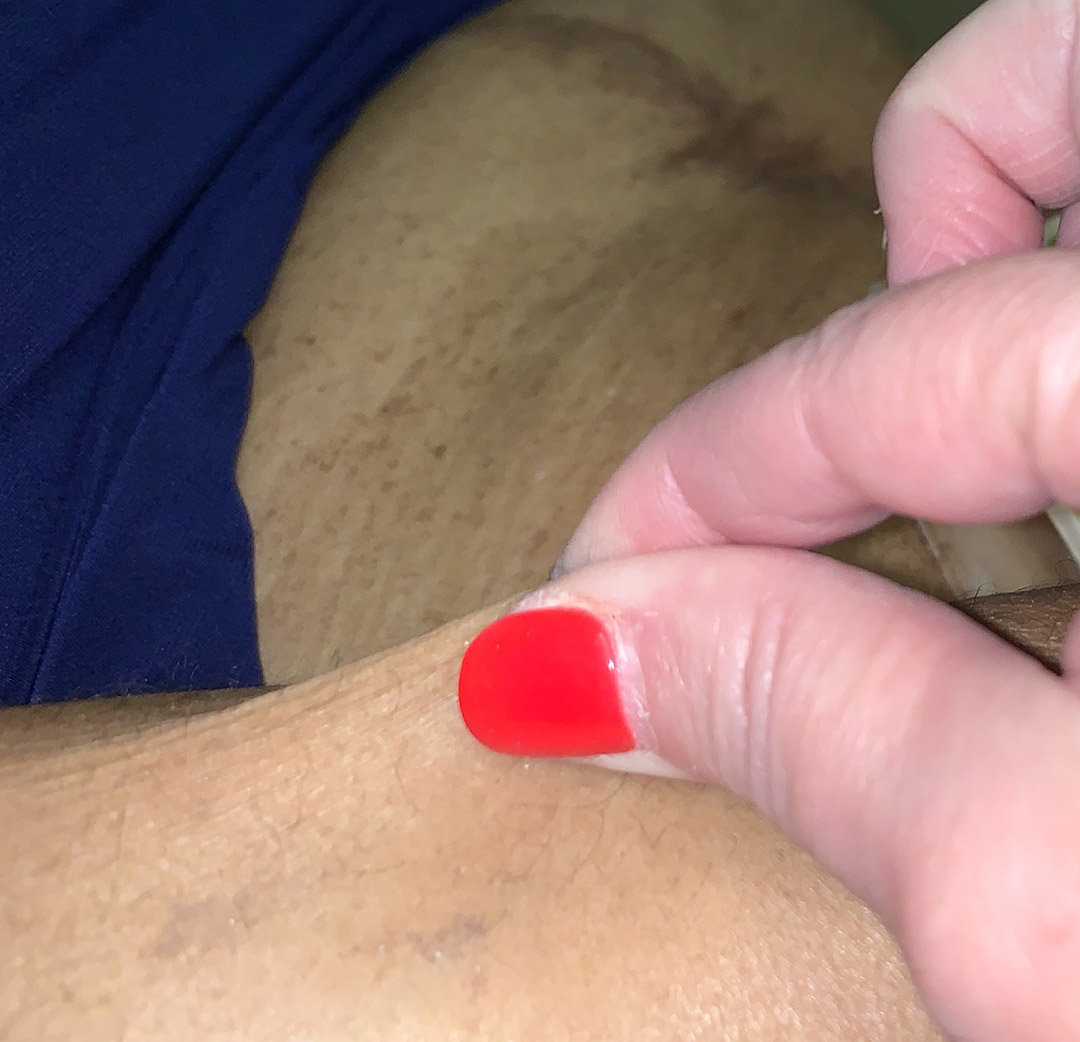
Note her rubbery skin, which is far more flexible than the laxity associated with old age, and the characteristic parchment-like scars. How many cases of EDS have I have missed in 30 years if I have found 3 of this “very rare” condition in one year?

Dr. Fife is a world renowned wound care physician dedicated to improving patient outcomes through quality driven care. Please visit my blog at CarolineFifeMD.com and my Youtube channel at https://www.youtube.com/c/carolinefifemd/videos
The opinions, comments, and content expressed or implied in my statements are solely my own and do not necessarily reflect the position or views of Intellicure or any of the boards on which I serve.



Have one right now that had a massive hernia repair followed by flap closure that had a dehiscence and has required HBO, VAC, and a lot of TLC. Closing, but slowly. It wasn’t missed as it was known prior to the surgery.
What would you do differently to treat this wound if you had known the diagnosis prior?