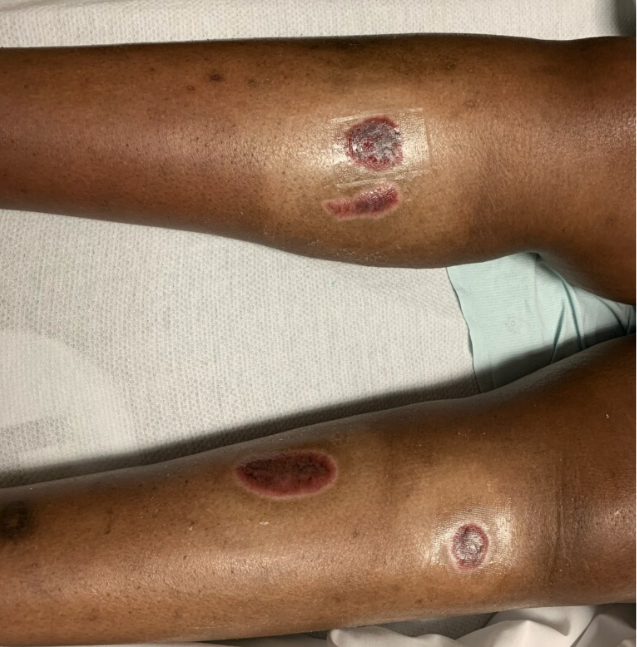
A few weeks ago we began an experiment right here on this blog, taking a look at a complicated wound care case and “crowdsourcing” the diagnosis. We thought it would be fun to share some of the comments to date, along with some follow-up comments from me.
Hopefully this will help us clarify the comments, drive the conversation further, and allow us to draw some conclusions. To be continued!
COMMENTS:
Although the patient is not on dialysis could be calciphalyxis
–Rob Snyder
Consider early exotic infectious illness triggered by steroids and stress (leishmaniasis, histoplasmosis and anaerobic soil organisms)
—Bill Palko-Schraa DO
Love the Diagnosis show!! Figure 1 is an App that is also terrific for crowd sourcing information. Pyoderma Gangrenosum? albeit not painful … occurs spontaneously … also have a similar case I’m looking at … Any drainage? debridement? is it superficial or full-thickness? hard to tell from photo … current treatment?
—Anita Prinz, RN, CWOCN
Behcet’s although no mucosal involvement necrobiosis is a valid thought that can be seen on H&E, not PG as that is neutrophil dependent peroxidase degranulation also seen on H&E…what does the peripheral blood smear look like, SPEP, procoagulant assays???
Similar organ failure history, sure there isn’t a Polycolonal agammagobulinopathy at play?? Or vasculidities??
Lymphoma from GVHD??
–Dr. Traci A. Kimball CWSP
What other drugs are they taking?
–Helen Gelly, MD
Reaction on the medication?
–Ann
How about Necrobiosis lipoidica?
–Philip Rettenmaier
Mycosis fungoides? Agree with Dr. Palko-Schraa to consider “zebras” here due to immunosuppression.
–Katie Cecconi, PA-C
Would obtain an incisional biopsy of two of the lesions. One piece of tissue needs to be sent for formal histopathology (& read by an experienced pathologist) and the second piece of tissue to be sent for PCR (see advice of an infectious disease physician).
–Deb Verran
Possibly due to inability to regulate inflammation. Grafts help modulate inflammation up or down. The graft will decrease the pain. Obviously a negative culture and path report can leave you wondering. But the patient wants that hole closed and does not care what label you place on it.
–Cheryl
FOLLOWING UP:
GREAT comments everyone! I thought I’d add a few clarifications from me based upon your questions and comments. Hopefully this can help drive the discussion. Comment away with your thoughts!
- Biopsies for pathology, read by a nationally-renowned Dermatopathologist, did not show anything useful (no pyoderma, no vasculitis, etc)
- Biopsies for viral, acid-fast and fungus were negative
- The lesions are not painful
- Oral steroids (starting at 40 mg daily) did not help
- Intralesional steroids did not help
- Topical steroids did not help
- A DNA assay is not possible because all 3 are all in-patients
To be continued…

Dr. Fife is a world renowned wound care physician dedicated to improving patient outcomes through quality driven care. Please visit my blog at CarolineFifeMD.com and my Youtube channel at https://www.youtube.com/c/carolinefifemd/videos
The opinions, comments, and content expressed or implied in my statements are solely my own and do not necessarily reflect the position or views of Intellicure or any of the boards on which I serve.