Doctors are supposed to be like parents and not have favorites. However, one of the best things about this field is that just when your attitude begins to flag, a patient comes along who reminds you why you got into wound care — or even why you got into healthcare. Many patients have inspired me, but Morgan holds a very special place in my heart. Yep, I said her name. I have her permission to talk about her -– and not for the first time.
I gave Morgan McCoy my own personal “Undaunted Spirit” Award, and was constantly encouraged by her attitude during the darkest days of COVID-19. She’s been a guest editor for Today’s Wound Clinic. Frank Aviles and I interviewed Morgan, her parents and her surgeon for a special “Wound Rounds” series sponsored by HMP – this one called “A Second Chance at life thanks to Courageous Choices” –- in which she talks about nearly dying from a necrotizing infection and undergoing an above knee amputation. (Her amazing surgeon, Dr. Kyle Dickson received huge criticism for NOT doing a hip disarticulation -– he wanted to give her the chance at an AKA -– as long as she got good wound care.)
The part of the story that we haven’t talked about is that, despite learning how to dance and kickbox with an AKA prosthesis, she’s continued to have a smoldering chronic ulcer on her medial stump due to pyoderma gangrenosum (PG). In fact, it was the PG lesion that told us her inflammatory bowel disease was still not under control. Now that her underlying problem is controlled, she is about to say goodbye to “Greg,” her chronic leg ulcer – after 3 years. I asked Morgan to tell me what she wished people understood about living with a chronic wound and her message is below.
Before you read what she has to tell doctors and nurses about living with a chronic wound -– Morgan’s personal “Brave and Strong” Day is Oct 14th. She celebrates the loss of her limb and the saving of her life every year by participating in a dance marathon to raise money for the Children’s Miracle Network Hospital. If you are feeling sorry for yourself for any reason, snap out of it – donate to Morgan’s fundraise and read her message here.
–Caroline
Things people should know about living with a chronic wound:
1. It takes work!
Daily dressing changes require a whole new time commitment to a daily routine. Depending on the situation, wound care can take up to an hour a day. Think of all the things a person could do with that hour of time, and how many total hours it adds up to, over weeks and months. I’ve probably spent over 1,000 hours on the care of my wound – more time than I spent in my hardest college or graduate school classes.
2. There’s a learning curve.
The wound care team see wounds all the time but it is probably the patient’s first time to see a wound — and it’s a totally different situation when it’s on your own body. It takes time to get comfortable caring for a wound. I appreciate my doctor when she tells me, “Don’t worry! You can’t mess this up!” about my wound care. I didn’t even look at my wound for months. I had my amazing parents as my caretakers to do my dressing changes until I was ready to see it. (You can see why I was afraid – below is a photo at my first wound center visit on December 17th, 2019). The wound team didn’t make me look until I was ready.
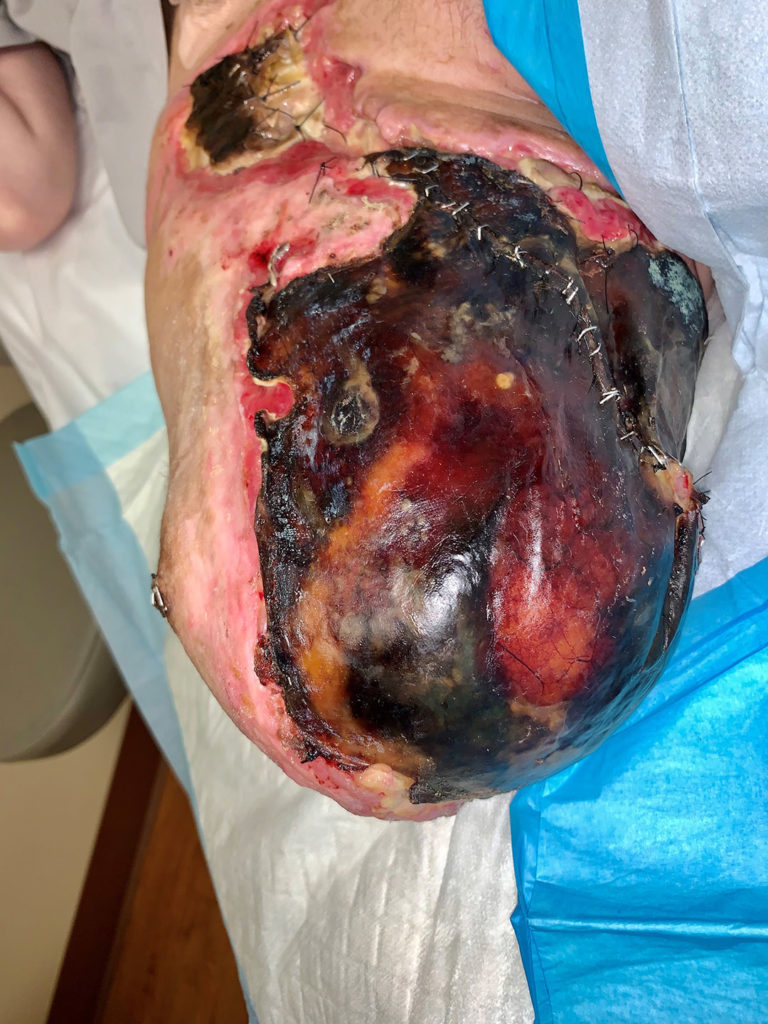
It’s okay to be afraid to look and take a break from thinking about your wound. It’s a process and learning how to be comfortable with wound care doesn’t happen overnight. Finding the right wound care setup takes time — creating a space that looks nice but has all the supplies you need right there where you treat your wound is key (this is a learning curve too, lots of trial and error). I had to have a dressing changing station in my dorm room – see below!

3. It’s emotional.
As wounds change, feelings change. It can be a rollercoaster. If you lose ground, it’s emotionally draining. And no matter what, a non-healing wound makes a patient feel like they are failing – even when it’s not their fault. If the wound is related to a traumatic event, caring for the wound can trigger powerful emotional reactions out of proportion to the situation. The tubing from my Negative Pressure Wound Therapy (NPWT) device reminded me about tubes coming out of me in the intensive care unit. I have a visceral reaction to tubes. Physicians need to understand that wound care is as much a mental thing as a physical one. Please give us grace and time to process. Please help us feel safe, heard and supported.
4. It limits your life… and often controls it.
It sucks when a wound prevents you from being able to participate in activities you love. For me not being able to swim was heartbreaking. I love being in the water, but it’s not safe to expose a wound to the bacteria that might be present in pools and oceans.
Having that activity taken from me means that the wound is controlling part of my life. That’s difficult and upsetting, particularly when some of those activities are the very ones that help you cope with stress. Helping patients find alternatives or compromises is helpful. For example, while I HATE the super sticky “drape” used for NPWT, sealing my wound and getting to swim in a chemically-balanced pool every now and then is a good compromise. That compromise gives me joy. I was allowed to start using a prosthesis while I still had a wound because the wound was not in a place where the prosthesis would put pressure on it. My team has always tried hard to help me participate in college activities despite having wound. I am grateful when the attitude is, “How can we make this possible for you?” rather than, “You just can’t do X .”
5. It requires a lot of trust in the team.
It’s easy to lose hope when a wound stops getting better (or gets worse). It’s easy to be mad at them and take frustrations out on them – even when you know they are doing their best and know that they want you to get well nearly as much as you do.
I want my physicians and nurses to know that my reactions are not personal. The emotional journey is hard and unfortunately sometimes doctors and nurses get the brunt of it. Give patients space to process. Physicians can help manage patient fear and triggers through communication- asking what they can do to make a patient feel safer or more in control of the situation during the visit. Being open to adapting your methods to help fit a patients’ emotional needs is key to gaining their trust.
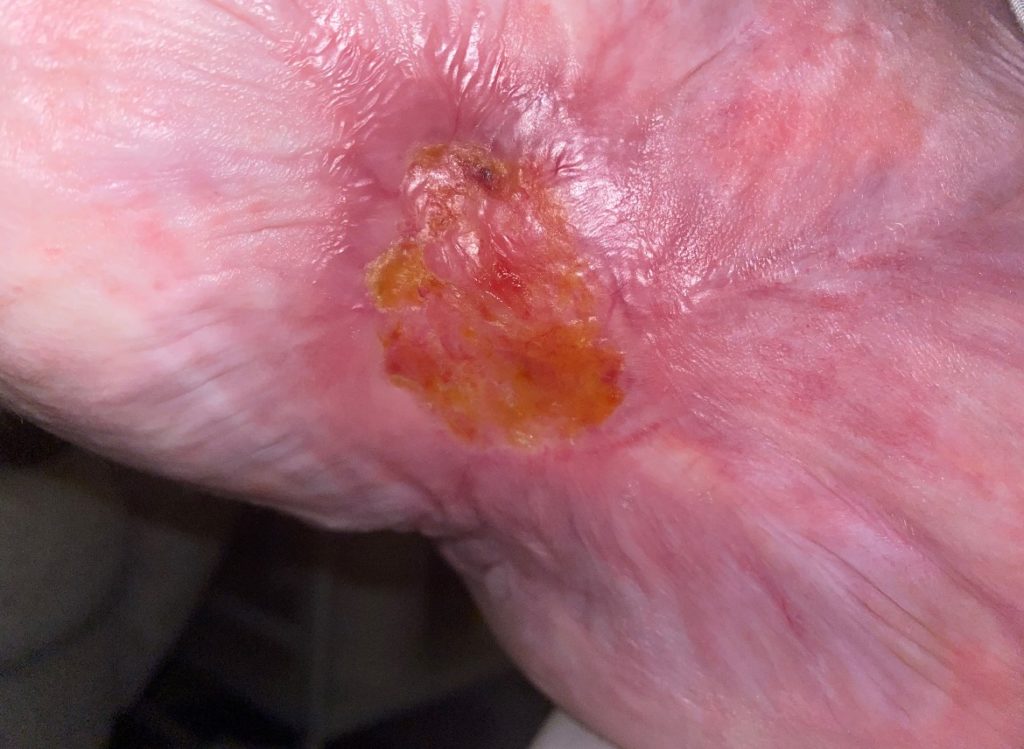
My wound is finally on the way OUT. When it’s gone, I will have to get used to NOT wearing a dressing and taking a normal shower! It will be a whole new kind of adjustment, even though it’s a good one. Every step of the wound care journey requires some adjustment -– even healing.

Dr. Fife is a world renowned wound care physician dedicated to improving patient outcomes through quality driven care. Please visit my blog at CarolineFifeMD.com and my Youtube channel at https://www.youtube.com/c/carolinefifemd/videos
The opinions, comments, and content expressed or implied in my statements are solely my own and do not necessarily reflect the position or views of Intellicure or any of the boards on which I serve.




Uhm . . . WOW . . . Thanks for sharing Caroline, but even more thanks to you, Morgan, thank you so much for sharing your ‘journey’ and getting Greg out of your system !
Excellent topic. Thanks for sharing. Also thank Morgan for her perspective and tell her hello for me.