I need your help. If you are a wound care practitioner, I need you to follow the instructions on my blog and download your “Non-pressure ulcer” Field Test report and have a look at it. I know that reading about this issue is like taking an Ambien, but stick with me and I will tell you why spending a few minutes to get your report could help save the field of wound care.
I fully support the development of a “cost measure” which would reflect the cost of the care among patients I care for who have chronic wounds and ulcers. Although I was originally board certified in Family Practice (FP), for 34 years I have practiced only wound care. Since wound care is not a recognized medical specialty, and since patients with chronic wounds are likely to see me more often than they see their primary care practitioner (PCP), Medicare thinks I am the PCP for all the patients I saw in the wound center. I was deeply concerned in 2016 after reading my “QRUR” (Quality and Resource Use Report) which showed that hospitalizations for wound center patients with heart failure were being attributed to my Tax ID number (TIN). Since more than 50% of patients with chronic ulcerations have heart failure as a comorbid condition, and since these patients are often hospitalized for CHF exacerbations, CMS was holding me accountable for failing to prevent their hospitalization. That could result in a “claw back” of my Medicare claims – for things that I had no control over!
Eight years later, Medicare is finally developing a “cost measure” for “non-pressure ulcers,” and that means all DFUs, VLUs, arterial ulcers, and the “nameless” chronic ulcers. If that measure is developed properly, wound care practitioners would be held accountable for the way they use Medicare resources in patients with chronic ulcers. That’s a good thing! If the cost measure is developed properly, we will be held accountable for costs totally outside of our control and the situation could be worse than being on the hook for CFH exacerbations!
Acumen is the Medicare contractor tasked with developing a “non-pressure ulcer” (NPU) cost measure and they are now testing the measure that they created. If you are a wound care practitioner who saw at least 20 patients with a chronic ulcer in 2021-2022, there is a field test report waiting for you on the Quality Payment Program (QPP) website. I need you to download it and read it. I need you to message me with your thoughts, or alternatively, email me the report and the associate Excel files.
I am still digging into mine, but the scenario below explains why it’s important. Remember that CMS genuinely wants to ensure that the costs a physician is held accountable for were actually costs under their control. That’s the hard part about this. I am going to skip the details about triggering codes and confirming codes and use the case below as an example.
Who are these doctors outside my TIN?
Table 4 of your report will be a list of the “Top Clinicians Within and Outside Your TIN Contributing to Your Part B Physician/Supplier Episode Costs.” My report lists 5 practitioners, and I did not recognize the names of any of them. I have never referred to any of these physicians nor have they ever referred a patient to me. Yet, they have contributed the most to my episode costs. How is that possible? Most of them are not even in my geographic area. I am confident that whatever costs they are associated with were never under my “reasonable control” and that the patient must have seen them outside of whatever care I was providing.
Of particular concern, Quest Diagnostic Laboratory was listed several times in column W as if it is a “clinician”, as is Southwest Regional Pcr LLC which is another laboratory. Why are laboratory services listed in column W as if they are “Clinicians?”
My most costly patient:
My most costly patient accrued a cost of $108,245.57. Using the date of birth in the Excel file, I looked up her medical records. My last visit with her occurred approximately 8 months before the end of the “episode of care” attributed to me. Thus, for more than 50% of her episode I had no physician-patient relationship.
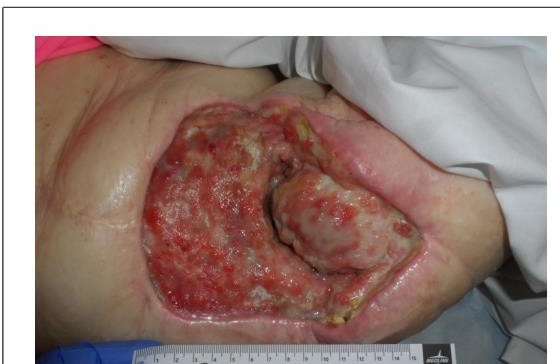
The patient had a large open wound to her right hip which exposed the hip joint following surgery for cutaneous calcinosis. She developed calcinosis as a result of high dose local radiation more than 40 years prior for a sarcoma. Long term survival of sarcoma patients is rare, and she underwent high dose radiation before fractionation. A year before seeing me, she underwent a wide excisional debridement of the irradiated field and then failed primary surgical closure in 2020. The photograph below shows her after she had improved dramatically. The photo depicts an open hip joint and the round structure on the right is the head of her femur. This chronic ulcer is more than 15 cm x 15 cm and extends into the pelvis.
She disappeared from the wound center and apparently became the patient of a nurse practitioner whose name I will not reveal. I do not know that NP, but she is the top clinician contributing to “my” Part B costs.
I looked up the NP and found that she is affiliated with a company which provides “mobile wound care” for the purpose of applying Cellular and/or tissue-based products (CTPs) in the home setting. As you can see, this massive wound would require many thousands of dollars of such products(inaccurately referred to as “skin substitutes”) which are not recommended to be placed over bone or open joints.
Here is what I have learned so far about the cost measure:
- Costs have been attributed to me for services ordered by an NP who saw the patient after I was no longer caring for her.
- The charges provided by the NP who cared for the patient were excessive and are attributed to me.
- Calcinosis and late effects of radiation should be excluded from the cost
Now I need you to look at your report and email me at cfife@intellicure.com. We need to get this right.
The comment period closes on March 14th, 2024.

Dr. Fife is a world renowned wound care physician dedicated to improving patient outcomes through quality driven care. Please visit my blog at CarolineFifeMD.com and my Youtube channel at https://www.youtube.com/c/carolinefifemd/videos
The opinions, comments, and content expressed or implied in my statements are solely my own and do not necessarily reflect the position or views of Intellicure or any of the boards on which I serve.



