I need your help. If you are a wound care practitioner, I need you to follow the instructions on my blog and download your “Non-pressure ulcer” Field Test report and have a look at it. I know that you are already thinking, “blah blah blah” and I don’t blame you. However, here’s another example of how problematic this report is. We have until the 14th to provide feedback to CMS about the “Field Test.”
Check Out My “Non-Pressure Ulcer” Field Test Report! (and download your own!)
My Second Most Costly Patient
My second most costly patient accrued a cost of $74,367. I looked up this patient using his DOB. The patient had advancing necrosis of the toes on the right foot and increasing rest pain (despite diabetic neuropathy) in the setting of diabetes and chronic renal failure on dialysis. The ischemic changes of the foot had been getting worse for several months after a podiatrist nicked his toe when clipping his toenails. He had already undergone both surgical and endovascular revascularization, as well as surgery for a large abdominal aortic aneurysm and aortic valve replacement. He had previously been hospitalized at a skilled nursing facility for generalized weakness and repeated falls. Arterial screening performed in my office with skin perfusion pressure showed a flat pulse volume recording indicating that he had no capillary flow to the foot. His foot was cold, and his toes were ischemic. No further vascular interventions were possible. He was destined for a foot or leg amputation and the goal was to keep him as comfortable as possible, but he was not a candidate for hospice.
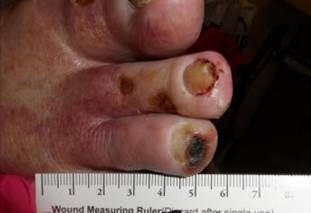
He had an ischemic foot on his initial visit. Photos below show the progression of the ischemia over a one-month period of time. He went on to amputation the following year.
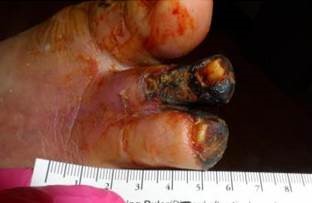
His major comorbid conditions include diabetes with renal failure on dialysis, advanced peripheral arterial disease, ischemic heart disease status post coronary bypass, sleep apnea, frequent falls, heart failure, depression, anemia, a right bundle branch block requiring a pacemaker, malnutrition, esophagitis, and autonomic neuropathy. His risk score is only 1.26. How is that possible?
Here is what I have learned from this case:
- There is a serious problem with the way that risk is determined and this needs to be looked at carefully.
- Patients with diabetes on dialysis and who are doomed to an amputation will create cost outliers. Failing to adequately account for this situation will make physicians reluctant to provide care to these unfortunate individuals.
- Costs are being attributed to me which are outside of my
I Might Have an “Episode” Myself Before This is Over . . . .
The problem really lies in the way that the “episode” is calculated. I compared the last day I saw each of the 55 patients in my report with the start and stop of Medicare’s official episode of care. Of the 365 day episode that Medicare calculated, I was NOT following these patients (on average) for 343 of those days! In other words, 94% of the charges in each episode occurred outside of my control. To be clear, it’s not that I didn’t care for the patient(s) and it’s not that I wasn’t responsible for charges. In fact, in some cases I’d cared for patients for MONTHS. The problem is that the “episode of care” attributed to me was not the time frame during which I was seeing the patient!
Other Issues
Two of the five “top spending” practitioners are podiatrists (and they are podiatrists who do not refer to me nor I to them). I would like to understand how and if their use of CTPs (over which I had no control) contributed to my Part B costs. Additionally, in reviewing my report, I found the Directors of two other wound centers in my list of physicians. This indicates to me that the patient visited more than one Wound Center during the episode of care. This may represent the patient getting a second opinion which is totally fine! I often recommend that they do that. However, it appears if the patient saw me first, all the costs accrued by another wound care practitioner are allocated to ME. Think about what that would mean if Medicare started clawing back your money because another wound care practitioner is outside the norm on spending. Yikes.
We have until March 14th to give CMS feedback. Please folks. Don’t sleep through this one.

Dr. Fife is a world renowned wound care physician dedicated to improving patient outcomes through quality driven care. Please visit my blog at CarolineFifeMD.com and my Youtube channel at https://www.youtube.com/c/carolinefifemd/videos
The opinions, comments, and content expressed or implied in my statements are solely my own and do not necessarily reflect the position or views of Intellicure or any of the boards on which I serve.



