About Dr. Fife
Dr. Fife is a world-renowned wound care physician. She is the CMO of Intellicure, Inc., Exec. Director of the US Wound Registry & Editor of Today’s Wound Clinic.

Report Honest Healing Rates
It’s time for Wound Care physicians and providers to stand up for truly honest outcomes and transparent quality reporting. If we don’t we may see our entire profession wiped out. Click here to read more.
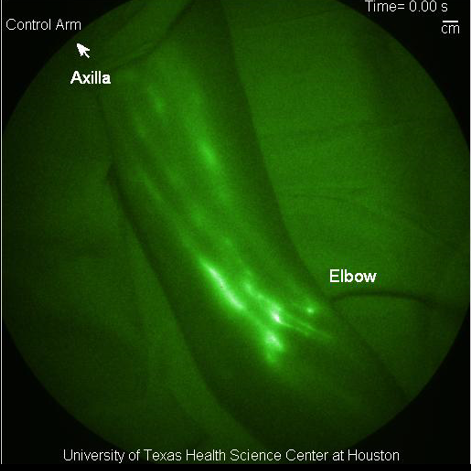
Guide to the Lymphatic System
A series of articles to summarize more than two decades of work in lymphatic imaging. Click here to read more.
Latest Posts
Overzealous Medicare Audits
Federal Investigators Probe Wound Care Industry – ClearHealthCosts
A New Review Article on Pyoderma Grangrenosum by Dr. Alex Loayza!
New Taxonomy Codes for Wound Care Practitioners!
This Might Be the Worst Flu Season in 15 Years
FDA Approves Suzetrigine, a Novel, Non-Opioid Drug for Moderate to Severe Acute Pain
Cellular Tissue Product (CTP) / Skin Substitute Sales Reps Needed! $9 Million a Year Potential in Commissions!
Don’t Miss the Alliance of Wound Care Stakeholders Webinar Feb 12th on the 2025 Medicare Final Rules!
Incisional NPWT Study Failed to Show Benefit After Surgery for Trauma-Related Lower Limb Fractures
Another Article from Clear Health Costs – is Patient Harm Happening in Wound Care?
BREAKING NEWS: Wound Care Company Owners Plead Guilty to $1.2 B in Fraudulent Claims for Amniotic Products and Face Prison
How Much About Access to Care With “Skin Substitutes” is Around Cost (and Will the LCDs Actually Make That Better for Patients)?
No End in Sight for the Spiraling Cost of Amniotic Products
Clear Health Costs Investigates the “Skin Substitute / Cellular Tissue Product” market
Breaking News! LCDs Delayed Until 4/13/25!
MIPS Basics – Watch it on Today’s Wound Clinic
Will Implementation of the Skin Substitute LCDs Be Frozen for 60 Days?
Landmark Antitrust Settlement Calls for Blue Cross Blue Shield to Pay $2.8 Billion into a Fund Designated for Physicians and Others
JAMA Patient Information about Obesity Medications
Proposed LCDs Raise Questions About ABNs That I Can’t Answer
Free Webinar Jan 16th, 2025: Clinicians Can Learn How to Submit Claims in the $2.8 B BCBS Antitrust Settlement
Slide Deck for the December 20, 2024 CGS Education Webinar on the Soon to Be Implemented “Skin Substitute” LCD
The US Cellular Tissue Product (CTP) / Skin Substitute Market Reached $1.75 Billion in the Third Quarter of 2023, Based on SmartTrak Analysis
Random Thoughts About Off-Label Drug Use and the Delphi Consensus Statement Process
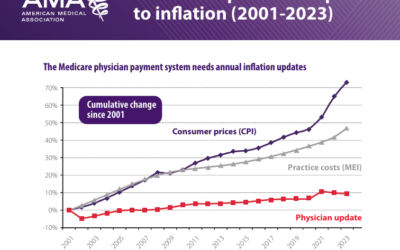
No Fix in Sight for the 2.83% Medicare Physician Pay Cut
Closing Year Thoughts
Compared to the Third Quarter, the Cellular Tissue Product (CTP) / Skin Substitute Market Grew 64% in the Fourth Quarter of 2024
The opinions, comments, and content expressed or implied in my statements are solely my own and do not necessarily reflect the position or views of Intellicure or any of the boards on which I serve.